Posted by Kathryn Gunnison, MD (a third year OBGYN resident from Kaiser Permanente, Santa Clara while on…
Global Health Elective: Nicaragua – PINCC – Laura Abbott, MD
Written by Laura Abbott, MD (a third year Obstetrics & Gynecology Resident at Kaiser Permanente, San Francisco while on rotation with the Kaiser Permanente Northern California Residency Global Health Program in Nicaragua with the PINCC Foundation.)
Global Health Elective: Nicaragua, PINCC
During the week of May 23rd to June 1st, I spent a week in Kukrahill – a small community on the Atlantic Coast of Nicaragua – working with Program International: No Cervical Cancer (PINCC), which is an organization that seeks to teach providers how to do cervical cancer screening that will be self-sustaining. To reach Kukrahill, you need to take a series of flights from San Francisco to Managua, then a separate flight in a 12-seater plane to a town called Bluefields, followed by a short taxi ride to the wharf and a boat ride to Pearl Lagoon, which is where the team was staying for the week. Kukrahill itself was another boat ride away – one that took approximately 20 minutes morning and evening. After arriving on the docks, we would all straggle up the hill to the small hospital where we ran a clinic to teach cervical cancer screening using Visual Inspection with Acetic Acid (VIA).
The night before we went to Kukrahill – the first trip PINCC had made to this location, and therefore unpredictable – we all met for dinner and an orientation. Our group was composed of 4 clinicians, including myself, who would be teaching those nurses and doctors who had volunteered to be trained in this method of cervical cancer screening. In addition, we had Carol – the organizer of the trip who was the perfect combination of calm, thoughtful and resourceful while also being something of a task master, in the loveliest way possible. We were accompanied by four support people, two of whom were RNs and two who were in some way affiliated with health care – one by marriage and the other through research. Two of the gynecologists had also brought spouses and children, who were there on vacation. Going into the week, we all felt a little like a rag-tag band, and I was personally nervous about what I was really bringing to the experience, given my limited knowledge of this particular type of cervical cancer screening.
That first day, we arrived in a boat riding low in the water because of the bags we brought with us. We had suitcases full to bursting with equipment, the most important of which included such simple things as white vinegar, cotton balls, q-tips, lubricant gel and headlamps. A cryotherapy gun was carried in a small brief case, and the real victory of that first day was having managed to get a tank full of nitrous oxide all the way from Managua to Kukrahill by bus (a local physician helped with transport, and the whole endeavor was three to six months in the works), but we also needed one of our support people to sort out how to fix the leak in the tubing between the tank and the cryotherapy gun, which was a proud moment for one of the non-physicians.
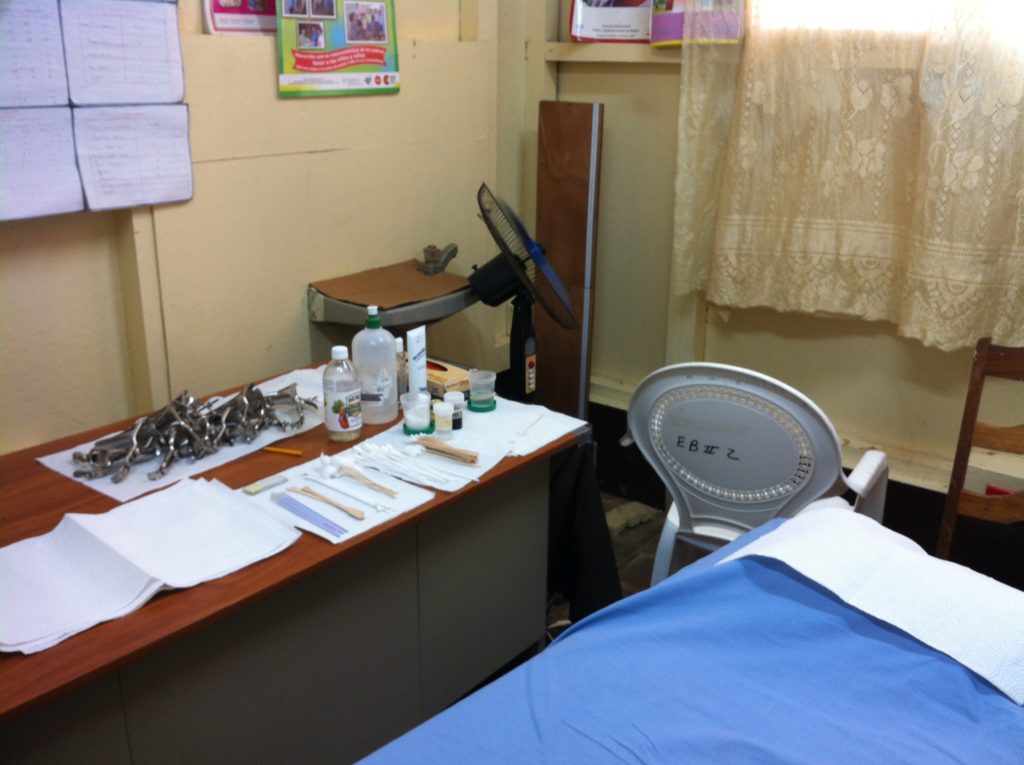
We started with a quiz that all trainees needed to take, followed by a lecture to teach the principles of VIA. After that, we split up and headed to our respective rooms. I was paired with a Spanish-only-speaking obstetric nurse, and our exam table was simply a wooden table with a drape over it. We made a make-shift gynecologic exam table using a chair to hold one leg and another table to hold the other, as there were no stirrups to be had. And then, we got to work. We had asked to start with a lighter day of 15 to 20 patients. Approximately twice that number showed up, and we still managed to see them all as we struggled to sort through the paper charts, screen the women (in Spanish) and teach our trainees the principles of VIA – identifying the anatomy, assessing for lesions, discerning between subtle changes that were abnormal and those that were normal. At the end of the day, we cleaned up and had a second educational session to review the answers to the tests they had taken that morning and look at images of cervical lesions.
At the beginning, the level of knowledge among the trainees was varied, but none of them had been exposed to this particular technique of cervical cancer screening. Most relied on Pap smears, but too many of the Pap smears were lost in transit to the nearest pathologist, and too few women actually returned to get the results. Therefore, there was a clear benefit to teaching these trainees how to perform a screening test that could give immediate results and would allow for immediate treatment in some circumstances or more rapid treatment in others. On my first day, with our first patient, I was somewhat disheartened when my trainee did not realize on physical exam that the patient had undergone a hysterectomy. It seemed that we had a lot of work to do over the course of just five days.
I remember our last morning, however – the electricity had gone out the night before and still was not back on when we arrived. We stood in a slightly dimmer room without any fan to push away some of the stillness of the humid air or help whisk away some of the sweat that accumulated in the 90-degree weather. We leaned over the patient, examining her by the light of our headlamps, and my trainee had clearly learned so much. She was able to identify far more of the changes we saw, distinguishing between precancerous lesions and the normal changes that occur with aging. There were still errors from time to time, but many fewer than on arrival. And, in re-taking the same quiz they had taken that first day, everyone in the group did significantly better. There was a real sense of accomplishment as we sat around in the group, expressing thanks for the time spent and the opportunity to work together to improve women’s health.
During my time in Kukrahill, I learned a great deal, even while I was teaching. I learned how to better describe the lesions that I saw, and I was able to perform procedures for the treatment of low- and high-grade lesions. More than that, however, I learned a great deal about how to implement sustainable teaching strategies that will allow for the future independence of providers in developing countries. I have long believed that the best way to help people in less fortunate circumstances is not through aid so much as teaching, because it is not just a band-aid or a quick fix but a way to continue to provide the same care even in the absence of such groups as PINCC. The same screening can continue without us, although PINCC will return in 6 months to continue teaching and to re-screen any of the patients found to have more minor lesions in the intervening time. Eventually, PINCC will certify these trainees, and they will continue to screen patients on their own. This is an amazing thing to give to other providers.
My time in Nicaragua offered me more than just the opportunity to learn and teach cervical cancer screening. It was a grounding experience, and one that reminded me of why I chose this profession and what really matters to me. Moreover, I was given the opportunity to meet and work with an amazing group of people who shared my interest in promoting the health of women everywhere and preventing the development of a very serious and often fatal form of cancer – a cancer that is almost completely preventable. The time spent with PINCC was quite short, but incredibly meaningful. I returned to the United States with a renewed sense of purpose and a better perspective on the challenges faced by those who have fewer resources – be they in Nicaragua or here, where not everyone has the same access to care or opportunities for follow-up that we so often take for granted.










This Post Has 0 Comments