Written by Hamad Zafar, DPM, PGY-2 at Kaiser Permanente Santa Clara Podiatric Surgery Residency Program while on Global Health rotation…
Da Nang, Vietnam – Tina Saparia, MD
Written by Tina Saparia, MD (A third year internal Medicine Resident at Kaiser Permanente, San Francisco while on a global health rotation in Da Nang, Vietnam at Da Nang General Hospital and Da Nang Orthopedic and Rehabilitation Hospital.)
I am a third year internal medicine resident at Kaiser San Francisco and was the fourth Kaiser Internal Medicine Resident to participate in this particular rotation. I was in Da Nang, Vietnam for a total of three weeks and split my time in three different departments: Orthopedics and Rehab Hospital, the Intensive Care Unit, and the Department of Cardiology. My experience is detailed below.
Da Nang Orthopedics and Rehabilitation Hospital –
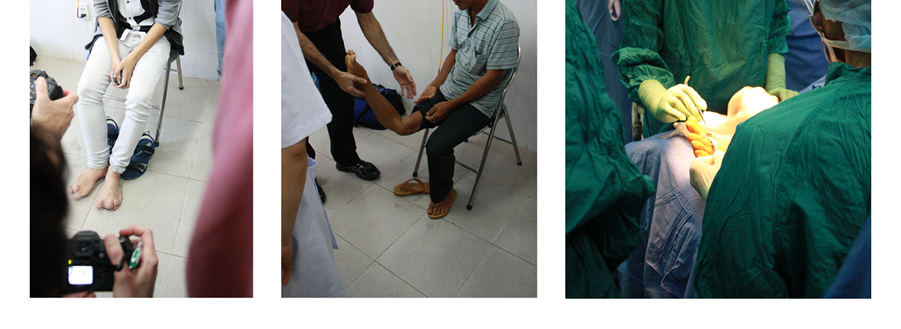
I just so happened to arrive to Da Nang around the same time as a large group (about 6) of podiatrists and orthopedic surgeons, from the Bay Area, both attendings and residents. One of the Kaiser-based podiatrists, Dr. Kaschak, also happens to be the main liaison between Da Nang’s hospitals and this Global Health Program (read a post from him here: http://kpdispatchesfrom.org/tag/da-nang-orthopedic-and-rehabilitation-center/). Dr Kaschak invited me to spend my first few days with their team which—though not at all my area of training—turned out to be a fascinating experience. The first day, we spent the entire day in clinic, where we triaged about 50 patients, from infants to the elderly, who had any leg or foot deformities. They had advertised this free clinic on the television, radio, etc and people from near and far waited all day to be evaluated for possible surgery. These surgeries would be performed by the American surgeons during the next two weeks, with plans to train the local residents and surgeons with new techniques. I saw all sorts of interesting pathology, including residual deformities from war trauma, polio, club foot, and congenital deformities.
Quickly, it was decided which patients would be operated on (about 30-35 patients), and the OR schedules filled up, starting the very next day. The following day, I spent in the OR, watching and even helping with some of the surgeries. I hadn’t been in the OR since my third year of medical school so I was a bit nervous, but the surgeons were so welcoming and enthusiastic to teach. In fact, they even welcomed my husband (who is not in the medical field but accompanied me for the first week of my trip) to come into the OR and observe some of the surgeries! It was incredible how efficient they were with surgeries and the minimal tools and monitoring with which the surgeries were performed. Two side-by-side simultaneous surgeries occurring in one OR room and with only one anesthesiologist? Never seen that before! I was also surprised to hear that post-op, these patients typically receive only acetaminophen or ibuprofen for pain control! Despite this, the patients and their families were so very grateful for this service, and truly seemed willing to go through just about anything to get these life changing procedures done so they could have the chance to walk again. Even post-op, when you would imagine they would be in so much pain, the patients showed nothing but good spirits and beaming smiles.
Intensive Care Unit – During the time I spent at the Ortho Hospital, the folks at the General Hospital around the corner finished up my paperwork, and by day 3, I was able to get started in the Intensive Care Unit. This is where I spent the next 1.5 weeks. The schedule is about 7am to 5pm, with an afternoon “siesta” style break from 11:30am to 2pm—incidentally also the hottest part of the day with temperatures reaching 110-112 degrees Fahrenheit!
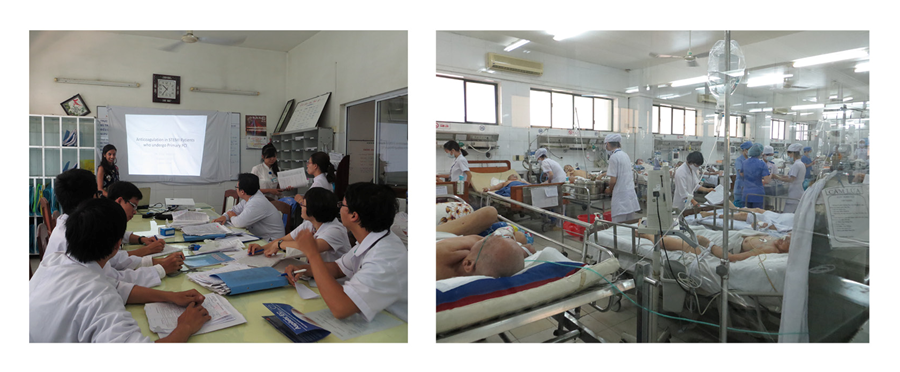
The ICU is a very busy department, with 60 beds, and is almost always at all full capacity. There are no residents in this department. In fact, completing a residency program is not required to be a doctor in the ICU. The team consists of about 15 doctors, some fresh out of medical college (which is a total of 6 years post high school education), and some seasoned intensivists who have been practicing many years. The chief of the department is a very animated person, who loves to teach and ask lots of questions. At 7am, we would begin with quick bedside rounds on the new overnight and sickest patients, followed by a meeting where the doctors who were on call would discuss all the deaths and admissions from the previous night. Then the doctors would finish their notes, write orders, and attend to any active patients in the unit. I didn’t always understand what was going on, as rounds and all discussion occur in Vietnamese, but luckily some of the doctors spoke some English and were able to translate for me. Although access to certain medications and treatment modalities may have been limited, the physicians seemed to always be aware of the latest guidelines and recommendations. I can only imagine the frustration of having the breadth of knowledgeto help a patient but lacking the physical resources to do so. The physicians and I exchanged management ideas with each other, and we often discussed discrepancies and similarities in management and referenced articles when appropriate.
During my time in the ICU I also got to partake in several procedures, including thoracenteses, intubations, and subclavian central line placements. There seemed to be an unusually large number of patients with COPD (smoking rates in Vietnam are through the roof) and strokes (both ischemic and hemorrhagic). And of course as with any ICU, there were also a lot of sepsis cases; in addition, it seemed that nosocomial infections were a major problem in this hospital. I also saw several poisoned patients from suicide attempts, as well as cases of severe Guillain-Barre disease, pre-eclampsia, myasthenia gravis, cerebral venous thrombosis, meningitis, snake bites, and Fugu fish (tetrodotoxin) poisoning. During my time rotating in the ICU, I gave presentations to the group on sepsis and infection control in the ICU.
I found it interesting to see how important of a role the patient’s families play in the care of the patient. Although only allowed to see their loved ones during certain restricted hours of the day, the families were responsible for feeding, bathing, and cleaning the patients, and were even responsible for running to the pharmacy to purchase necessary medications and supplies if not readily available in the ICU. Sometimes these family members would be teenage children of the patients; it intrigued me how much responsibility these young family members had in the care of their loved ones. Also, there is no such thing as “code discussions” or discussing end-of-life issues. Doctors are required by law to do “everything that can be done” for a patient. This can get complicated because it’s also part of the Vietnamese culture to be able to pass away in one’s own home, so getting a very sick terminal patient back home in a way that is legally allowed can be tricky.
Cardiology Department – I spent my last week in the cardiology department, which happens to be one of the largest departments at Da Nang General Hospital. It consists of about 120 patients. All patients with history of any cardiac disease get admitted to the department of cardiology regardless of admission diagnosis. So there were patients with UTIs, strokes, pneumonia, etc. admitted to this department, in addition to the typical STEMIs, NSTEMIs, endocarditis, heart failure, valvular disease, and other cardiac pathology. I was surprised to see that none of these patients had any form of continuous monitoring. In fact, in this department is where I witnessed a code blue with no cardiac monitoring and minimal equipment.
The chief of the cardiology department, Dr. Lai, was an incredibly warm and welcoming individual; also very smart and interested in teaching. He took me for one-on-one bedside rounds and teaching, where we examined various patients together and he told me what they were admitted for. He also showed me his favorite techniques for echocardiography and let me practice on a few patients in the unit. In the afternoons, we would spend some time doing treadmill EKG stress tests for patients with chest pain. I also had the opportunity to tour the echo suite and watch some cardiac catheterization procedures.
On one of the evenings, Dr. Lai invited me to his private general clinic in his own medical office. I had never seen anything like this before! Operated only by himself and his pharmacist wife, the clinic was equipped with everything from an ultrasound machine, EKG, lab draws and machines, x-ray, and even a dark room to develop the films immediately after. No nurses were present to help with these procedures; Dr. Lai would do it all on his own! And the patients he would see were of all ages, presenting for any type of problem. Despite having to do everything himself, we saw about 15 patients in the two hours I was there.
On my last day in the cardiology department, I presented several review articles on STEMI management to the cardiology team of physicians and medical students. That evening, the chief of cardiology and the rest of the department took me out for a dinner celebration.
People
By far, the BEST part of my trip to Vietnam and this Global Health Elective was the people I met while I was there. The Vietnamese, especially those in the city of Da Nang, were some of the most incredibly friendly and welcoming people I have ever met. Despite the language barrier, their hospitality was extraordinary. The doctors would often take me out for lunch or invite me to go out for dinner or coffee after work. I even met some of the physicians’ families and children. And oftentimes when I was eating alone at local restaurants, local families would shyly start up a conversation with me in their broken English and by the end of our meal we’d become friends.
Transportation
While personal cars are less common in Da Nang, what they call “moto-bikes,” or scooters, are extremely abundant. Traffic signals—absent. In fact, if you come to a full stop, chances are you will cause an accident. And how many family members can you spot on a single moped? I frequently saw up to five! As you can imagine, all this made crossing the streets quite scary, but with some practice, I got used to it. The trick: just walk into traffic calmly and the scooters will somehow make their way around you (or so you hope)! Although visitors can actually rent these scooters for a very cheap rate, I did not dare operating one in that traffic, though I did ride on a few as a passenger. I mainly got around by taxis, which were quite prevalent and relatively cheap.
Weather
The worst part of my trip was probably the intense heat. Being accustomed to the cool and foggy San Francisco weather, dealing with temperatures of 100+ degrees Fahrenheit and humidity at 100% was definitely taxing. Most parts of the hospital did not have AC (I can only imagine what it must have been like for the sick patients!). I mitigated this as much as possible by staying well hydrated, wearing cotton clothing to help keep me cool, and avoiding direct exposure to the oppressive sun as much as possible.
Accommodations
I stayed at the Brilliant Hotel along the Han River and loved my experience there. It’s a very modern hotel with great amenities, a beautiful view of the river, and close to tons of restaurants, bars, cafes, and shops. It’s also only about 1 mile from the hospital.
To do nearby / Sightseeing
As mentioned above, there are many restaurants and bars in the area. There is also the large and famous Han Market near the hospital and located along the river, which sells various local produce and merchandise. In addition, the beaches of Da Nang are absolutely beautiful and only a short 10 minute taxi ride from the hospital area. There are also several nearby towns that are worth a visit, including Hoi An, Marble Mountain, Lady Buddha, Hue, and MySon Sanctuary. I took a weekend trip with my husband to the city of Hanoi and spent a night on a boat cruise in Ha Long Bay, which was absolutely beautiful (I would definitely recommend this).
Food
Being a vegetarian, I found the food to be a bit of a challenge. It was difficult to communicate my dietary restrictions to servers at many local restaurants, so often I was limited to only vegan restaurants or places that were catered specifically to Westerners. That being said, I definitely enjoyed tons of delicious fresh fruits that were in season including mangoes, dragon fruit, rambutans (spiky, alien-looking lychee fruits), pineapples, and avocados.
Overall Experience
I am so glad I decided to do this Global Health Elective, and if possible, I would definitely do it again. It allowed me to see how medicine is practiced in another part of the world with its unique cultural norms, technological limitations, and practical realities. I will cherish this experience and am truly grateful for the people I met along the way. I highly recommend this rotation to other medical residents!


This Post Has 0 Comments