Written by Hongyu Zhao, MD, PGY-2 and Qing Meng Zhang, MD, PGY-2 at Kaiser Permanente…
Patient counsel- Searching for cultural sensitivity
8/17/12
Posted by Amanda Thornton, MD (a third year Internal Medicine resident from Kaiser Permanente, Oakland while on a global health elective in Lusaka, Zambia with University Teaching Hospital).
I’d mentioned in past blogs that since I cannot draw blood or do some of the medical history taking work that the medical students do because of the language barrier, I’ve been working on patient counseling. There are still a lot of pit falls for someone as American as I am- though I am not without sensitivities. I can tell when I have said something wrong, but often I am at a loss as to what it is.
Some of the time, patients are confused by my attempts to initiate the free-flowing interaction between patient and physician expected in American medicine. Here, physicians take a much more paternalistic approach- a kindly father, but still the authority with significant amounts of power. I have been told by Dr. Yumbe that patients’ reticence to enter into an open conversation with physicians is left over from Zambia’s colonial period, where any questioning of authority would be met with immediate loss of status, financial power or job status.
My parents, from their experience here in the 80s, also added that no one is willing to go into the intricacies of having other obligations for their money and when certain relative luxuries (compressive stockings for ladies with swollen ankles for example) cannot be afforded. The residents have been filling in the prices for many of the procedures, medications and laboratory tests that patients must fund- and even though I can translate into American dollars by dividing by 5,000 (which is a dreadfully awkward number)- I don’t have the fine understanding of what each profession makes and what one can reasonably expect one’s family to raise which would allow me to push certain treatments as cheaper or affordable.
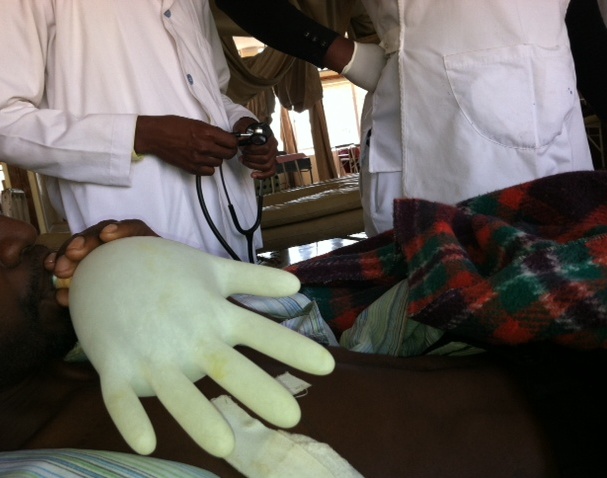
It really is ingenious the kinds of things that they use here at the hospital as cheap alternatives to expensive medical equipment. For example, a patient with pneumonia in the U.S. is given an incentive spirometer. But here, a patient showed me the version the nurses and physicians had come up with (pictured below with permission of the patient).
Still, my lack of familiarity with many aspects of life around here does make it more difficult to give appropriate advice- I have to look around at the faces of the listeners to figure out if they can actually take the advice I’m doling out and then readjust if it can not be taken or doesn’t seem well received. Usually, if I’ve been nice and approachable enough, someone will tell me why something is not feasible.
For example, there is currently a shortage of blood from the blood bank at the hospital. I was (very) surprised to discover this is because the schools are out of session- according to the intern on my team children as young as 10 years old can donate blood and stock the blood bank- my host here says she has only seen blood drives in colleges, where the population is over 18 . In a country where HIV is as prevalent as it is here, persons who have the possibility of being sexually active have greater risk of contracting HIV and donating blood in the undetectable period- where viral load is high but seroconversion has not occurred (and tests to detect infection may be less accurate). Logically, a younger age makes sense, though recruiting heavily in schools continues to make me nervous. I think the minimum age for blood donation in the U.S. in some states is 16 (in the UK it is 17) and there is also a weight and a blood count requirement, but here in Zambia, there are not as many healthy people to donate.
Still, when a patient presented with dysentery and Hemoglobin of 2.8… there are very few solutions other than blood transfusion. A hemoglobin of 2.8 is lower than I have ever seen before coming here- the normal range is 11-18 (the exact ranges vary by age and gender). I have to admit, I was surprised he walked into the filter clinic at all… I have never seen grey gums on a living person before looking in his mouth. We had been told by the blood bank that there was absolutely no blood available and to suggest that patient’s friends or family donate blood specified for patients. However, when I suggested that to the patient, he admitted that he was HIV+ as was his wife who was willing to donate for him. Even though her blood type was appropriate, to further complicate matters he was on antiretroviral treatment, but she was not- the risk of mixing a wild-type HIV with one treated is not one the blood bank would take or I would recommend. He asked me if he could pay anyone to donate for him or if it was possible to buy blood anywhere.
In the U.S., when blood banks were stocked by paid donation, the rate of infectious complications of blood transfusions were much higher, and that is one of the reasons donations are all voluntary now. Even though I am unaware if that is the case here, I told him it was safer to have a volunteer. He said there was no one other than his wife, and family members whose HIV status he did not know and could not politely inquire. I told him I would try to figure out what to do, and took the problem to the intern and then we took it to the attending who had a friend in the blood bank and managed to get blood for our patients with the lowest hemoglobin levels that night. A lot of things work by friendly connections here- everyone befriends lab technicians, nurses and orderlies who might be able to work the system when our hands are tied- and sometimes I think our patients are lucky that our team is so personable.
Some kinds of counseling are intrinsically difficult- and usually reserved for doctors specializing in psychiatry or psychology in the U.S. We had what seemed to be to be an excessive amount of suicide attempts in the filter clinic- though when I asked my resident, she shrugged and said it seemed average to her. It was time to work on another one of my weaknesses- since the toxicology screens are not rapid around here and there is no toxicologist on call- the clinical signs of poisonings (whether ingested or from animal or insect venom). Around here the poisons of choice for suicide (or homicide when added to beer, as apparently occurs relatively frequently), are either rat poison (warfarin- causes severe bleeding 24-48 hours after ingestion) or insecticide (usually containing high levels of organophosphates which severely weaken nerves and eventually lead to coma and death when ingested in large quantities).
Since I have gotten a reputation for effective counseling (though I strongly suspect that this is based solely on my available time and lack of other blood drawing and IV placing talents), I was directed to counsel a young woman and her husband after a suicide attempt. The patient would be discharged via psychiatry, but we wanted to make sure that the attempt would not be repeated. They had recently lost a newborn- and I struggled to get the patient to speak to me at all.
At least partially, I can blame this on culture- talking about death at all here is taboo. Late on our call night, nursing called for a (dreaded) “change in status” consult on a patient in the intensive care unit with new onset Cheyne-Stokes breathing. When we arrived, I recognized the colloquially termed “death rattle,” the sound made when saliva accumulates in a person’s mouth when he is no longer swallowing. After we reviewed the case which had several indications of severe organ dysfunction for which there was no solution, I asked if the patient’s wife at the bedside was aware of the seriousness of his condition and when the nurse questioned her (she spoke the tribal language of the patient’s wife), she was not. I asked if we should discuss the possibility that he might pass overnight, at the least to encourage family members to assemble given the seriousness of the situation, and my resident was aghast. I asked if we discussed palliative care (given that I have seen a few patients from hospice centers as well, and I know that not everyone is treated aggressively) and my resident said it was tricky, and typically not brought up by physicians.
While I think that discussing it might, at the very least, decrease the volume of the wailing and sobbing from the entire assembled family that occur every time someone passes (one of my hosts did a eerie mimicry of the exact sound which made me realize that it too is regional), I have recognized in families who have immigrated from other countries and from American families when discussions are unwelcome, and given my relative cultural ignorance I didn’t push the matter further. Besides which, I felt that directing the nurse to tell the patient’s family that the situation was grave and the solutions were few would at least give them warning. I was gratified to find (when I checked on the patient the next day) a small crowd of family members at the bedside.
However, in the case of a patient with a suicide attempt, there is no way I could imagine to have an effective discussion without speaking of death. At least, the fact that Zambia is a “Christian” nation helped- I could at least tell the patient to ask for support from church, friends and family- which would be overwhelmingly pro-life given the culture. But I don’t typically inject religious leanings into my patient discussions, the thing I probably did the most naturally was offering sincere sympathy and empathy- reflecting on the difficult time they had had and how important it was to keep as busy as they would have been with their newborn had it survived. I watched their faces to know when I’d given them enough of an idea of what might help and added that this was well within the natural mourning period and that if the feelings did not start to lift in the next few months, they should return without hesitation.
In the U.S. – I admit- I would have tried to do more of an assessment of their belief system as it would have have had more variability. But here, there is more homogeneity in some things, and hopefully the more directed approach was the most effective one.