Written by Hongyu Zhao, MD, PGY-2 and Qing Meng Zhang, MD, PGY-2 at Kaiser Permanente…
University Teaching Hospital – Maureen Cho, MD
Written by Maureen Cho, MD (A third year Obstetrics and Gynecology Resident at Kaiser Permanente, San Francisco while on a global health rotation in Lusaka, Zambia at the University Teaching Hospital.)
As a third year OB/GYN resident at Kaiser Permanente San Francisco, I feel so blessed to be part of program that gives us the opportunity to explore and expand on various aspects of medicine that peaks our interest outside of our daily hospital experiences. I love to travel and immerse myself in different cultures. With my devotion to obstetrics and gynecology, I hold a particular interest in understanding the diseases and conditions that affect pregnancy and female health in different parts of the world, and more importantly, the diagnosis and management of such diseases and conditions in these parts of the world where resources are limited. Through the Kaiser Global Health Program, I was given an opportunity to participate in an elective rotation with the OB/GYN department at the University Teaching Hospital (UTH) in Lusaka, Zambia.
Lusaka is the capital of Zambia with the city’s population totaling around 2 million people. UTH is the largest hospital in Zambia and serves as the main referral center for tertiary level of care for the entire country. It is also often regarded as “the best government funded hospital available in Zambia.” It is also the main site for medical education and training for doctors, fellows, midwives and nurses. The entire medical campus consists of over 1,500 hospital beds with subspecialists available in almost every aspect of medicine.
Flying from San Francisco to Lusaka, Zambia was one of the longest journeys I have ever been on. After 30+ hours of travelling, I finally stepped foot into Lusaka International Airport where I then stood in line for about 2 more hours to obtain my visa. Finally, I met my gracious host who took me to their home where I stayed with their family and a variety of other students/volunteers who were also living there while in Zambia for research, foreign exchange programs, etc.
I loved my peaceful stroll to UTH every day. Living far from the city center in a suburban neighborhood close to the President’s house, traffic was never too busy and the environment was always safe. I always took the back road lined with trees and nicely manicured lawns around privately owned homes. The main road was always more treacherous and chaotic with uneven pavement and dirt flying past you as cars whizzed by. My first day at UTH, I was greeted by Dr. Mwahanamuntu, a senior consultant in OB/GYN who was extremely involved in resident and post-graduate training. With Professor Parham, a gynecologist oncologist from the US, they pioneered the Cervical Cancer Prevention Program around Lusaka and other more remote areas of Zambia using telemedicine and trained medical staff to “see and treat” cervical dysplasia, while referring those with suspected cervical cancer to UTH for surgical or radiation treatment.
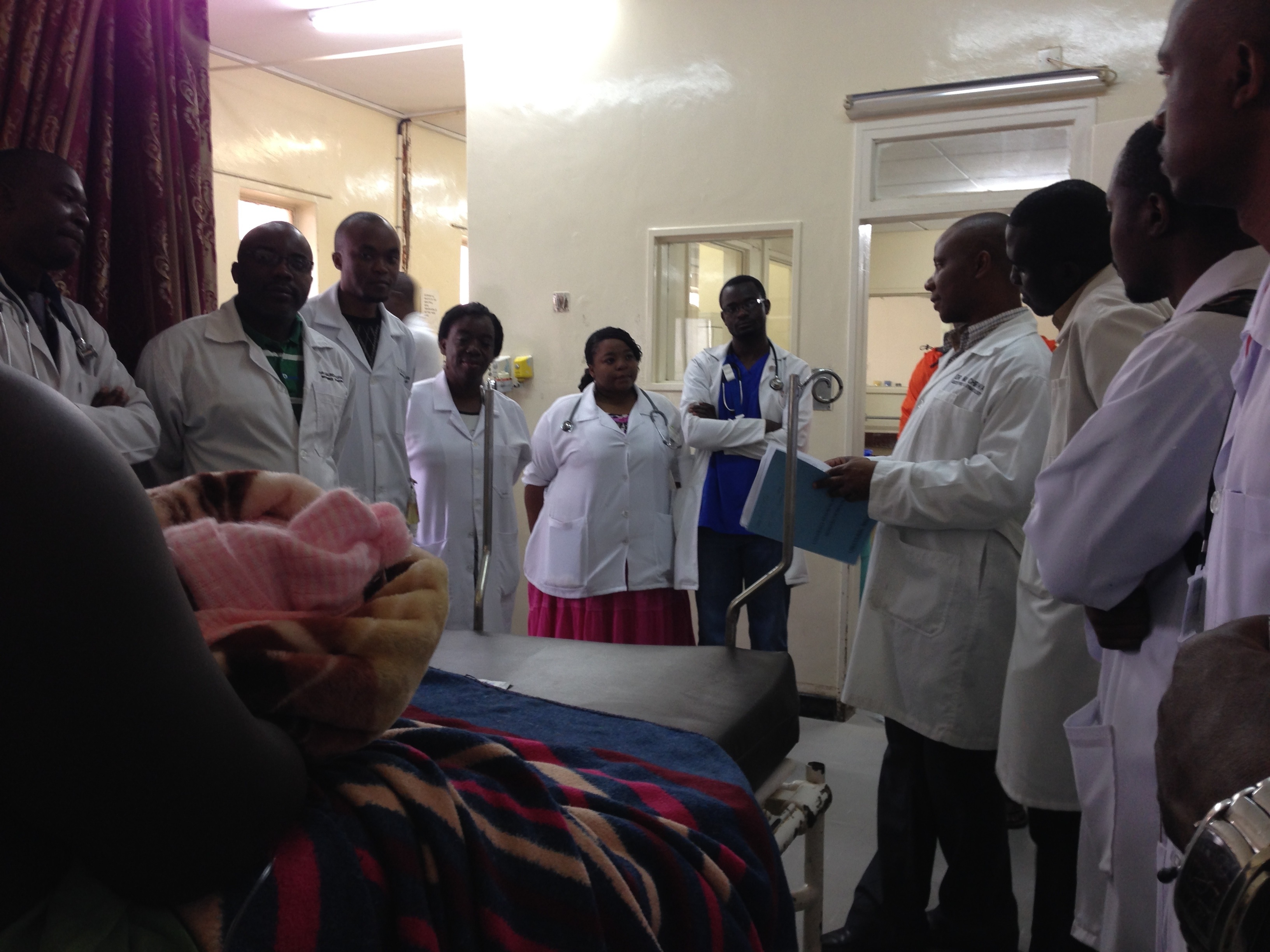
From day 1, I joined Dr. Mwahanamuntu’s firm and performed the hospital duties that his fellow residents and post-graduates did. Each firm had at least 10-15 physicians present of varying levels—interns, junior medical officers, post-graduate doctors (which was what I was equivalent to), junior registrar, senior registrar and ultimately the senior consultants. Each firm switched duties on a daily basis, which included outpatient clinic, major OB or GYN rounds, GYN surgery and 24 hr call which meant covering all of Labor & Delivery, GYN urgent care, and all obstetrical and gynecologic inpatients. On a given 24 hr day, there are typically 50-60 vaginal deliveries, 10-15 cesarean deliveries, 3-5 exploratory laparotomies, and 15-20 manual vacuum aspirations. As for triages, about 70-80 obstetric patients and 30-40 gynecologic patients are evaluated each day. With the high volume of patients, the only way to see everyone is to “divide and conquer.” Amongst the members of the firm, often the more senior post-graduates and junior registrars would take over responsibilities in the operating room, less senior post-graduates would round on the floor and laboring patients, and the junior medical officers and interns take over the L&D and GYN triage. The senior registrars and senior consultants are typically available by phone, but periodically would pop in on surgical cases or round on various inpatients at their leisure. When on call, I had the autonomy to split my time between these different areas to satisfy my educational desires.
What I took away most from this elective was that the appropriate management of patients and standards of care are entirely dependent on the resources available. What I have learned as “evidence based medicine” is not applicable and sometimes even inappropriate even in a teaching hospital of a major city depending on the part of the world you are in. Nonetheless, the physicians there continue to strive to give these patients the best care and attention they possibly can. This is where I learned that making the “right” decision for the patient does not always lead to a good outcome because of events that are out of their control, such as planning for surgical management of an acute ruptured ectopic pregnancy when the one functional OR is backed up with 6 emergency cases. Encounters like this gave me a very real perspective of the struggles that both physicians and patients face on a daily basis.
Labor and delivery is located on the second floor of a very old building. Lighting is dim, furniture extremely worn out and sparse. The unit is littered with laboring women in any free space one can find. When all 14 beds are filled, thin foam mattresses are laid along the walls of the hall and onto the floors of open shared 4-person rooms. Each patient brings their stack of delivery supplies: one or two pairs of sterile gloves for the doctor, several “chitenge” cloths that are first worn as a skirt, then unwrapped from their body and draped over the bed to serve as a bed sheet and absorbent pad since linens and disposable drapes are almost non-existent in the hospital, one towel to wipe the baby after birth, a set of baby clothes, and one or two packs of cotton fluffs that the doctors and nurses break into various sizes to assess for bleeding, clean the patient after delivery, or serve as a maxi pad. Laboring women that do not know each other lie next to one another within inches away from each other on mattresses lining the halls while awaiting a laboring bed to free up or for the OR nurse to take them to the operating room for their cesarean delivery. With only a handful of windows providing ventilation, the stale air always smells of a mixture of sweat, blood, bodily fluids and dirt.
One day, while rounding on laboring patients, I heard a woman scream from the hall. I ran out into the corridor and found a young woman in a squatting position staring down at her small baby, no more than 5 lbs, that delivered spontaneously onto the ground, surrounded by a puddle of fluid, umbilical cord still attached, both mother and baby stunned with no cries heard. I was in shock and quickly put on some sterile gloves as I approached the scene. I had no towel, no clamps, no scissors—just my gloved hands. The post-graduate/resident assured me that things were fine and that it happens almost every day as I was still digesting the scene. Some nearby laboring women laid there watching, while others paid no attention and continued to cope with their own labor pains. Several minutes later, the midwife came with a towel and some instruments, and the day continued as nonchalantly as could be.
I continued rounds on the remaining laboring patients with the resident. Barely an hour had passed since the previous hallway delivery when I heard a lot of commotion in the halls again. I walked over to see what was going on and saw a woman lying flat on her back with labored breathing, her legs spread open with two little feet sticking out in between. Frantic, I asked why this patient was in the hall, and one of the staff responded that she had been waiting several hours already for her cesarean delivery. There were no laboring beds available to move the patient to, and the patient was screaming in pain with every contraction. I called for the other resident, and the junior registrar also happened to walk by at the right moment. With the three of us together holding her legs back and coaching her through her pushes, I experienced my first singleton breech delivery. Thankfully mother and baby did wonderfully and went home that same day. These experiences really showed me how hard the doctors try to make the right medical decisions for their patients, but sometimes in the end, the events that we had hoped to avoid still occur out of their control. I compared my “tiring” 24 hr shifts as a resident at my home institution to theirs, and I feel that any complaints from me are unwarranted compared to the workload and challenges that they face every minute of their day. I truly admire their stamina and passion to advocate for their patients, and hopefully one day will make positive changes to the standards of care for the women in Zambia.
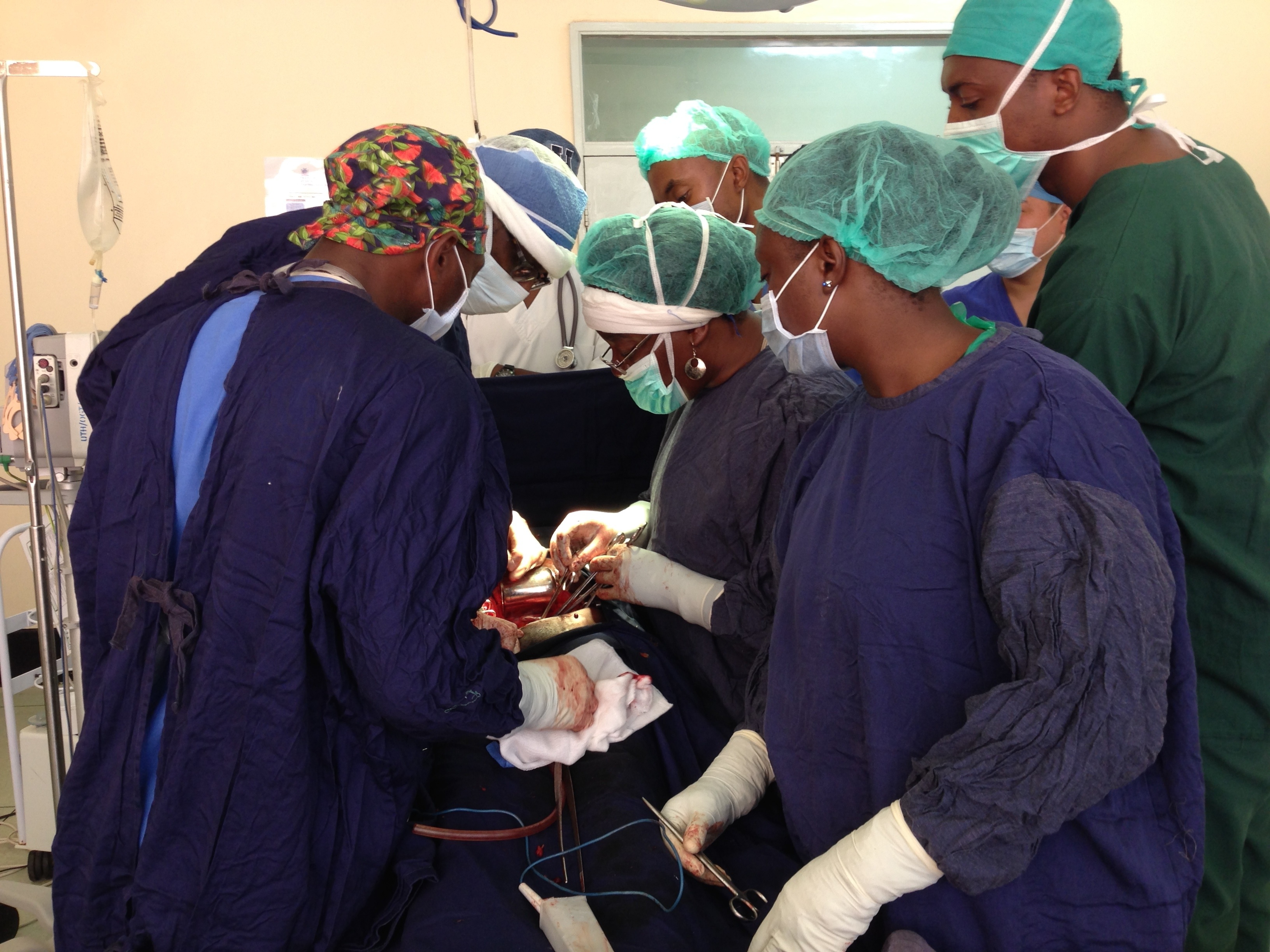
My experience in Zambia was so fruitful that I can talk for days about the interesting cases I saw like malaria in pregnancy, abdominal tuberculosis, missed diagnosis of gestational trophoblastic neoplasia, as well as surgical challenges I experienced firsthand, like performing cesarean deliveries with only a limited number of instruments that were extremely blunt, using a syringe needle to cut the umbilical cord after vaginal deliveries, performing LEEPs without a colposcope, performing radical hysterectomies with a standing gooseneck lamp raised by stacked stepstools… and the list goes on and on. But the story I want to end with is of a patient that has touched my heart forever. Ms. K, a healthy 30 year old woman just became a new mom to her beautiful baby girl. Besides a long labor course, her vaginal delivery was uneventful and was discharged home on postpartum day 1. Two days later, she was readmitted to the hospital with abdominal pain and fevers, then developed sepsis from an infection in her uterus. She was hospitalized for 1 week, treated with IV antibiotics and ultimately discharged home recovering well. Over the next several days, she noticed a rapidly growing abdominal mass with occasional bouts of mild pain, but otherwise no significant symptoms. She came back to the hospital 4 days after being discharged home and was found to have a large, well-circumscribed, firm abdominal mass comparable in size to a 34 week pregnancy. Ultrasound was unable to discern what type of mass this was, and CT imaging was expensive and would take at least 2 days for results to return. Regardless of our inability to determine a definitive diagnosis, exploratory laparotomy was recommended to determine what the mass was and to remove it in order to avoid further complications given its rapid growth. She broke down in tears and begged not to be taken to surgery. She was afraid. The senior consultants explained to her that surgery was necessary while she was still stable and that she would be fine. Her eyes looked at us with doubt and insisted not to be taken to surgery. I put my hand on hers and told her that it was okay to be afraid. I told her I knew she was worried about her baby, but we needed to make her healthy again so that she could be the strong, healthy mother that her baby needed. I looked her in the eyes and told her that she was a very brave woman, and we are all here to help make her healthy and well again. She let out a sigh, smiled and nodded. We scheduled her tentatively for surgery in 4 days and ordered a CT scan in the interim. However, over the next 1.5 days, the mass continued to expand remarkably, at which point she spiked a high fever, could no longer tolerate oral intake and appeared to be decompensating. After much pushing and shoving, we were able to get her into the operating room that night and found the mass to be a huge abscess filling her entire abdomen and drained 3 liters of pus out of her belly. There was so much inflammation and scar tissue that her pelvic organs were completely encased and unidentifiable. Parts of her bowels were denuded and required reinforcing stitches. At the end of the surgery, she was left with two drains in place and one long vertical incision down her abdomen. The next day when I went to see her, she was edematous and drained of energy, but her eyes lit up when she saw me with an ear to ear smile. She looked at me with such strength in her eyes, thanked me and told me that I was the one that gave her the courage to go through surgery because she really believed in what I said. I was so touched I didn’t really know what to say, so I just smiled and gave her a big hug. I was really taken aback because I never realized that my words could be so powerful and mean so much to someone. I saw her everyday while she recovered in hospital, met her lovely family and beautiful baby. To her, I gave her strength and courage, but to me, she gave me the confidence that I can make a positive impact in someone’s life, which is truly such a special gift that I hold dear to my heart.
What I have learned to appreciate when traveling abroad to experience medicine in a different country is to always keep an open mind and to respect the medical care that is given to the people of their country, which will always result with the most rewarding experience one could have wished for. Even though my contributions are limited at this point of my training, the amount of appreciation from the team at UTH and the individual gratitude from the patients further reinforces the potential impact that we can make even halfway across the globe. These are the types of experiences that continue to strengthen my interest in global health, and I am determined to continue my efforts in providing healthcare to those in need, one country at a time.



Great post. I was checking continuously this blog and I am impressed!
Extremely useful information particularly the last
part 🙂 I care for such info a lot. I was looking for
this certain information for a very long time. Thank you and best of luck.
Hi Maureen, I am going to be doing my elective at this hospital in obstetrics in March 2015. Just taking my final exams at Nottingham University in the UK. I am looking for somewhere to stay, do you have any recommendations or contacts?
Also can I get hold of PPP at the hospital if I need it? Or should I buy it here>
Would be so great to be in touch. Savanna Harrison UK
Hello, nice post, congratulations,
I am Asuncion Coves, OB/GYN resident in Spain,
I am interesed in external rotation in this Zambia Hospital,
Could I get your Mail to contact you.
Thanks!