Angkor Hospital for Children – Siem Reap, Cambodia – Meg Rothman, DO
Posted by Meg Rothman, DO (a third year Pediatric resident from Kaiser Permanente, Oakland while on a global health elective in Siem Reap, Cambodia with Angkor Hospital for Children).
Angkor Hospital for Children (AHC) — Siem Reap, Cambodia
and The Lake Clinic — Tonlé Sap Lake, Cambodia
Posted by Meg Rothman, DO a second year Pediatric resident from Kaiser, Oakland while on a global health elective in Cambodia
Angkor Hospital for Children : A Pediatric Teaching Hospital
I landed in Siem Reap, Cambodia on May 6, 2013 to volunteer at Angkor Hospital for Children (AHC). AHC is a nonprofit pediatric teaching hospital. It was founded in 1999 by Kenro Izu, a Japanese-American photographer who came to Cambodia to photograph the nearby UNESCO World Heritage Site and historical religious shrine Angkor Wat. His visit inspired him to do something to help the children of the area. Public health and medical care in Cambodia is burdened by the legacy of the country’s long history of war and political struggle. Many basic needs remain unmet: clean water, sanitation, education, transportation, and communication are unavailable in many areas of Cambodia, both rural and urban. Health care is provided by a network of government hospitals and clinics, NGO hospitals and private clinics. There are also traditional healers and lay midwives. The quality of care varies widely, and resources, even in the best hospitals, are limited.
Angkor Hospital for Children extends most of a city block on a vibrant commercial strip in Siem Reap. When I approached the hospital for the first time, I had to weave a path through a line of parked motorbikes and streetfood vendors. The perimeter fence is painted a cheerful green, and every gate is attended by guards. Inside I found an open play area where one young boy chased another across the concrete. As a pediatric resident, I felt an immediate sense of familiarity in this child-centered environment.
The hospital grounds comprise a thoughtfully laid out complex of pale yellow and white stucco buildings with red tile roofs reminiscent of buildings in California. The walkways, both indoors and out, are dotted with benches on which caregivers and children slept, ate, played, cried — and waited. An oral rehydration area stands near an outdoor triage station. In an adjacent cooking pavilion set up for families to use, pots of porridge bubbled, and free produce and nutritional instruction were provided. The facility maintains an outpatient clinic, inpatient ward, ER/ICU, OR, dental and eye clinics, physical therapy and social work departments. There is no dedicated neonatal unit, though plans to develop a NICU are being discussed. Surveying the landscape, I could see that AHC presented an overwhelmingly positive and functional environment.
AHC trains pediatric residents in a three-year program. Most attend medical school in Cambodia, although a few study abroad in places such as Vietnam, the Phillipines and Russia. Residents perform the same functions as residents in the United States; they round on patients, discuss plans with their attendings, write progress notes and orders, serve as the primary contact people for patients and families, and attend daily didactics. They work both day and night, maxing out their hours at about 60 each week. Like residents in the US, they forge close working relationships, drink caffeinated beverages (tea instead of coffee) to stay awake through the long hours and get sleepy during late-afternoon PowerPoint presentations. Many carry smartphones. The residents welcomed me and I felt at ease working alongside them. A pervasive attitude of calm kept stress at the hospital to a minimum.
My idea of what it meant to be a volunteer evolved over the month I was there. I learned far more than I contributed, which is what AHC expects. Rather than take the lead, resident volunteers are invited to observe, build relationships with Cambodian residents and attendings, and examine and read about patients and their diseases. As I engaged in these integrating activities, a sense of trust developed between me and the staff. Eventually, I was offering my clinical reasoning and doing some teaching.
I spent the first week in the inpatient department known as the IPD. It consists of a 30-bed open pediatric ward, two isolation rooms and a four-bed neonatal unit. At first, I saw the ward as a hot, humid cacophony of crying children. (The hospital is cooled only by fans, which means the temperature and humidity can reach 100-plus degrees with 85 percent humidity.) Most families come from remote rural areas, so they sleep at the hospital for the duration of the admission. A covered outdoor daytime waiting area doubles as sleeping quarters at night.
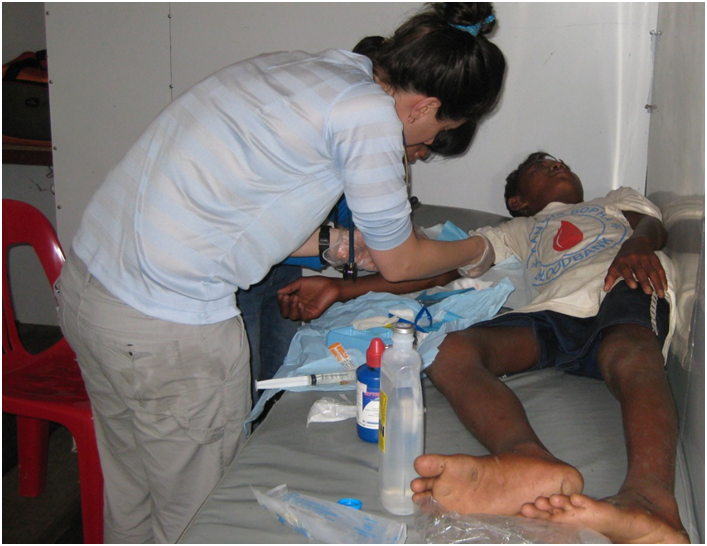
During my first few days in the IPD, along with rare congenital syndromes and life-threatening infectious diseases, I saw familiar pediatric problems such as pneumonia, asthma exacerbations and impetigo. Malnutrition and lack of access to routine outpatient care exacerbated these common pediatric conditions. A 9-month-old boy came in for a weeping and crusty whole-body rash. His mother had taken him to a traditional healer, who, as it was explained to me, had rubbed a medicinal plant all over his upper torso. His chest and back were abraded and infected. We cultured the rash and confirmed that it was staph aureus; the child had a severe case of impetigo. This was a severe presentation of a familiar diagnosis. Over the following days, his mother and father stayed with him in his isolation room, bathing him and keeping him calm. Gradually, with IV and topical antibiotics his skin healed.
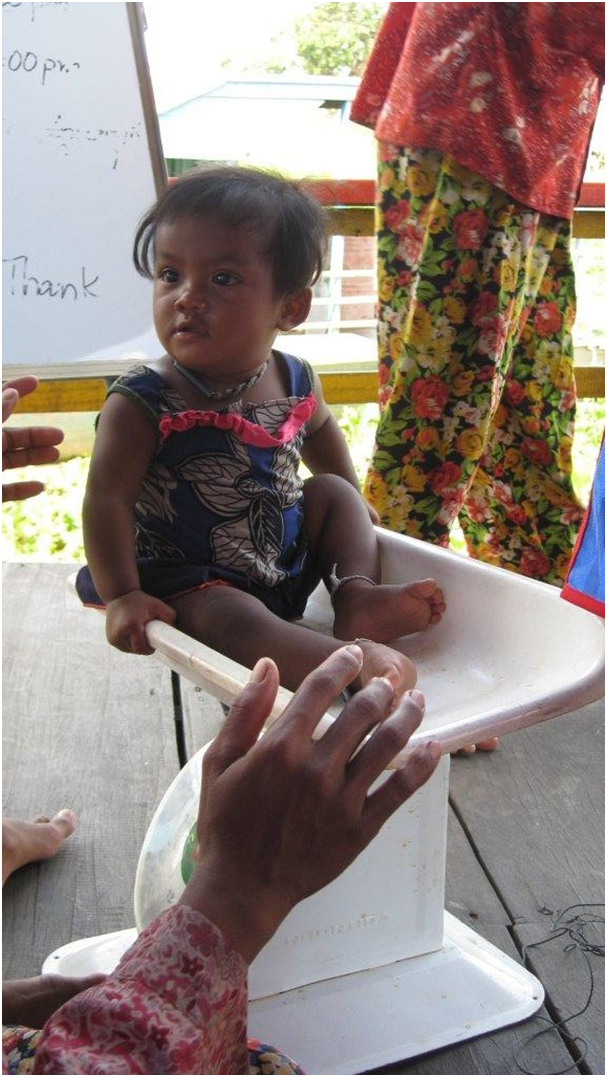
I met many patients with diseases I had never seen before. A 1½-year-old girl with severe malnutrition had been on the ward for three weeks when I first saw her. She weighed 5 kg and was severely developmentally delayed. I offered her the rainbow-colored metal bell of my pediatric stethoscope for exploration. She dropped the bell just as quickly as she reached for it, her wasted muscles collapsing under the weight. Despite treatment of her malnutrition according to World Health Organization standards, she struggled to gain weight. While in the hospital she had acquired and recovered from a respiratory viral infection and had intermittent diarrhea. She had gained and lost 100 grams here and there, but at the three week mark she was back at her admission weight. Her family, poor and from a rural area far away, had been living at the hospital during this time. Her mother took turns with her father at the bedside, as the patient’s 3-year-old sister ran barefoot around the ward throughout the day.
A 3-year-old girl with a trifecta of MRSA vaginitis, salmonella non-typhi septicemia and giardiasis was understandably miserable. Part of her treatment was topical vaginal Betadine three times a day. When I went to look for her in one of the few isolation rooms on the ward, she wasn’t there. It was common for parents to carry patients outside for a change of scenery. The nurse tracked them down in the cooking area. I approached her as gently as I could, starting with a cardiac exam. She screamed and kicked me.
I encountered patients with many infectious diseases. Two infectious disease I had not heard of before were EV-71 and Chikungunya disease. Chikungunya is a viral disease spread by mosquitoes. It causes fever and severe joint pain and potentially muscle pain, headache, nausea, fatigue and rash. Care is supportive and the disease is not usually fatal. The word “chikungunya” is derived from the Tanzanian Kimakonde language and means “to become contorted,” describing the stooped appearance of sufferers experiencing joint pain. EV71 is a common cause of hand, foot and mouth disease in children, and most patients recover within four to six days. However, severe neurologic complications, such as acute encephalitis and polio-like paralysis, can develop in some patients.
I was able to sit in on a hospital-wide conference similar to what we would call morbidity and mortality conference. A resident presented the case of a boy who had recently died at AHC after being treated for disseminated intravascular coagulation and shock. It was presumed that he had dengue hemorrhagic fever, an infectious disease for which the seasonal epidemic was just beginning.
While at AHC I met Claudia Tuner, MD, PhD a British research pediatrician and clinical microbiologist. I assisted with data collection for two of her current research projects, both involving retrospective record reviews. One study aims to identify the causes of morbidity and mortality for neonates admitted to AHC between January 2010 to 31st December 2012. The other aims to characterize outcomes of critical care transports between the AHC satellite clinic. I spent two days at the satellite clinic, in the rural village of Sotnikum, 35km from the city of Siem Reap, reviewing charts of critically ill infants. I was struck by how many times I came across a chart that was marked with the words ‘hopeless case’.
I spent much of my last week at Angkor Hospital for Children in the outpatient department, which sees 500 patients on a busy day. Space is limited and small examining rooms are sometimes shared by two physicians.
Part of AHC’s strategy is to defer the provision of primary care services, such as routine childhood vaccinations, to the government health centers when possible. Their aim is to avoid developing an NGO health care system that runs parallel to the public system. Instead they want to encourage the emergence of more comprehensive government health centers.
The hospital prohibits volunteers from taking photographs inside the hospital. AHC wisely puts patient and family privacy over the curiosity and interest of visitors. The photographs of AHC that accompany this blog are from an archive of photographs from past volunteers and staff. AHC does not offer tours of the hospital to the general public. Their policy contrasts with that of some local organizations, including some orphanages, which offer tours and photo ops to tourists and are considered by many to be exploitative.



The Lake Clinic
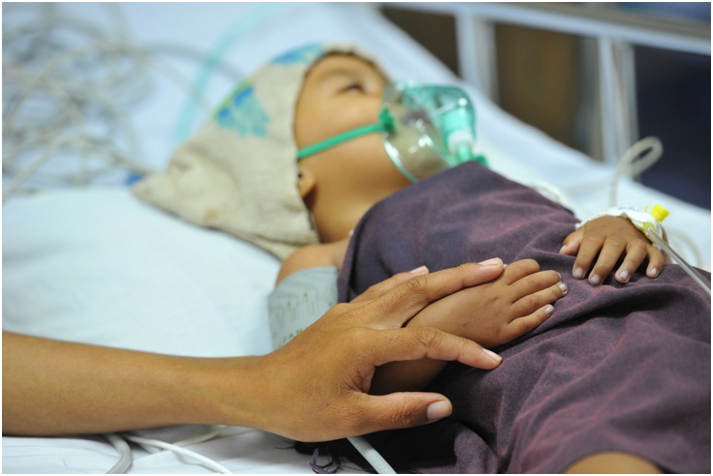
I also spent three days volunteering with The Lake Clinic (TLC), a floating/mobile health clinic that brings basic health care to people living on the Tonlé Sap lake. Aside from these periodic visits from the floating/mobile health clinic, these people do not otherwise have access to medical care – preventive or therapeutic. The Tonlé Sap is a combined lake and river system in Cambodia that is also the largest body of water in Southeast Asia. The surface area of the lake swells from 2,700 to 16,000 square kilometers during monsoon season. I traveled by van with the clinic team from Siem Reap to the village of Kompong Khleang, where we then boarded a boat. We cruised down a river of the same name to reach the Tonlé Sap Lake, eventually arriving at the floating village of Peambang. Here, we spent three days providing walk-in urgent care from The Lake Clinic (TLC). The medical team consisted of family physician Dr. Hun Thourida (Rida), pediatric nurse Uk Savaan and a midwife.
On our first morning, a 13-year-old boy came to the clinic seeking treatment for a puncture wound. At 3 a.m., while he was out fishing, a hook had caught his right upper arm and bit into his bicep. A heavy fish had been attached to the line at the time the hook punctured his arm. He was quiet during the examination, though he appeared to be in pain. I suggested a tetanus shot but quickly learned TLC doesn’t have the capacity to refrigerate vaccines and that it is prohibitively expensive for the patient to travel across the lake for an inoculation. Fresh blood seeped slowly from his wound, which was deep but only about 1 cm in length. Dr. Rida and I attended to the wound. We gave him wound care instructions and asked him to return the following week for suture removal. I thought about how hard it would be to keep that arm clean and dry in this environment.
Later that morning, a boat approached carrying two adults and two children. A man sat crouched in the front of the boat. He looked ill — very thin, with large sunken eyes and taut shiny skin. Our gaze locked for several seconds as the boat glided across the water toward the clinic. Although he was only 46 years old, he appeared to be 75.
The man had recently been discharged from a city hospital. He had no medications or medical records with him. Dr. Rida, who saw the patient, wasn’t sure exactly what he had been treated for. His heart and lungs sounded normal, and he had no fever. She was unable to perform any labs tests. That night, as I tried to fall asleep on a cot under the mosquito netting, a woman’s voice called out over a loudspeaker somewhere in the village. The sound carried easily over the water. For a couple of hours, she sang and chanted. A man’s chanting voice eventually replaced hers. In the morning, I learned the announcement had been a death notice. The 46-year-old man I had seen in the boat had died. Later that morning, I smelled the smoke from the nearby pyre as it drifted into the clinic.
Volunteering is a generous term to describe what I did in Cambodia. This was my first experience in international medical work. I knew nothing about the culture, did not speak the local language and had never seen many of the diseases the patients brought to us. As a volunteer it seemed that I took more than I brought. Angkor Hospital for Children invested in my education, and I can only hope that what I contributed in return was useful enough to make the visit worthwhile to my hosts. My month in Cambodia is already affecting my practice in Oakland. I know that physical exam is paramount. I am thinking about how to streamline my diagnostic process. I know I’ve been changed by this work and am grateful for the opportunity that it provided.