Mountain Volunteer – Nepal-Maureen Cho, MD
Posted by Maureen Cho, MD (a third year OBGYN resident from Kaiser Permanente, San Francisco while on a global health elective in Kathmandu, Nepal with Mountain Volunteer).
Reflection of my experience in Nepal
Nepal is a country like no other that I’ve been to. Kathmandu, the capital of Nepal, is home to roughly 3 million people and is the most urban city in their country. Walking the streets of Kathmandu, you get a true sense of what it is like to be in a developing country. There is one main road circling the city, which is one of the only road that is paved; however, there are no dividers on the road to form traffic lanes or even to separate the side of oncoming traffic. Traffic lights are non-existent. There is a constant haziness in the air from the inevitable dust and smog. Pedestrians do not have the luxury of walking on a sidewalk—you must keep your eyes darting between vehicular traffic and the ground you walk on to avoid cars and motorcycles from colliding into your path or tripping over the rubble, uneven stepping grounds and trash. Stray cows and goats share the road you walk on. Walking down the main road, you pass by many dilapidated buildings housing multiple families in a single room. Groceries are purchased from stands with rusted metal roofs held down by stone and buggy carts along the roads. Fresh fish and meat infested with flies are strewn across wooden tables. About every few miles, there are ditches with faucets protruding from brick walls with running water. Everyday, hoards of people are there washing their hair, their clothes, and always a line of people with big plastic or metal containers to bring their only source of water back to their homes. Almost all areas of Nepal, including rural villages, have access to electricity. However, the ability to generate enough electricity throughout the country remains a major issue. As a temporary fix, the entire country undergoes scheduled power outages daily. Being the central area of commerce in Kathmandu, power outages occur twice a day for 5-6 hours each time. Outside of Kathmandu, power outages can occur anywhere from 3 to 5 times per day for hours at a time.
Helping Hands Community Hospital is located within the center of Kathmandu. It is a private hospital that charges patients 50-75% less than the cost for medical services compared to other private hospitals. My first day there, I learned a great deal about their healthcare system and access to medical care. There are only several government hospitals scattered throughout Kathmandu and a few other major cities with virtually none that exist in the rural areas. There is no insurance system in Nepal, but fees for government hospitals are hugely subsidized so that the cost for services are very low and affordable, even for the lower economic class. However, the wait time for medical care is unreal and the conditions of the hospitals are well below par. Those that live in rural areas typically travel a day or two by foot, followed by another daylong bus ride or a flight into Kathmandu if they can afford it. In the emergency rooms, it takes days to be seen, and it is through here that the assessment must be made to determine if hospital admission is necessary. Once hospitalized, all medications and supplies including syringes, gauze, etc. must be purchased by their family members. For those that require surgery, family members must go to the blood bank and purchase 2 units of blood the day before the surgery. Sometimes it becomes a matter of cost that the family cannot afford, or a shortage of the patient’s blood type, leaving the family members literally crying and begging at the doorstep of the blood bank. But, obtaining blood products is only a minor obstacle. The hospital facilities simply do not have enough manpower and rooms available to accommodate those that require medical attention. Thus, the wait time for any surgical procedure can take days, months or even years. When I posed the question, “If a patient’s condition is evaluated to be serious enough to require surgical intervention, how can the patient survive waiting even days?” The doctor I asked shrugged and chuckled hesitantly, acknowledging that access to medical care is a huge problem for middle class citizens and below, but unfortunately, it remains the course for many people with many patients dying during this process. Those that have the financial means can go to private hospitals for faster access to care.

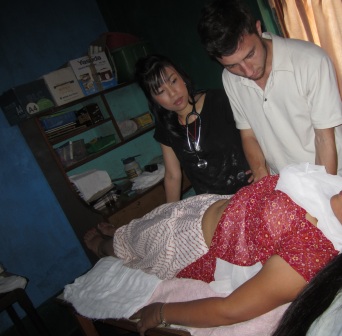
My experience as a gynecologist at Helping Hands Hospital was a huge eye-opener to the issues surrounding women’s health and the way medicine is practiced in Nepal. All of the physicians that serve at this hospital are all volunteer physicians that come and see patients either before or after their main responsibilities at their respective hospitals. Outpatient clinic hours vary between 2 to 4 hours daily with office times that change on a daily basis. The clinic consists of a single room with a metal sink, a desk, an exam table behind a curtain, and several stools. Patient privacy is not a common practice. There can be up to 3 patients in the tiny room at one time along with random family members—the attending is obtaining the history of one patient, the next patient is sitting in a chair waiting her turn, while I perform a pelvic exam on the patient we just interviewed behind the curtain. At most 5 minutes is spent on each patient in total, which leaves virtually no time for counseling. The patient virtually has seconds to ask the questions that she has before her opportunity is lost and our attention has moved on to the next patient. The attending writes a progress note in a paper booklet along with the recommendations (lab tests, prescriptions, etc.), which is kept by the patient. The hospital only has a registration log of when the patient was seen, but keeps no medical file of the patient. It is up to the patient to purchase the recommended medications from the pharmacy and perform the recommended tests. It is also up to the patient to return with their lab or imaging results to be reviewed by the physician. Definitive surgical treatment is often the recommendations of the gynecologists for fibroids, abnormal bleeding after completion of childbearing, pelvic organ prolapse, etc. When I asked why the patient is not counseled on the option for medical management, most attendings have told me that lack of follow up care is the main reason. Most women either will not return for follow up as advised due to cost of office visits, or they come from villages far away without easy access to pharmacies for medications and continued medical care. For those same reasons, as well as the lack of resources within the hospital to provide quick definitive diagnostic testing, many patients are over-treated for conditions that they likely do not have. For example, women that come in with a complaint of vaginal discharge and itching will often be treated for pelvic inflammatory disease, yeast infection, and parasitic infections, even if their physical exam findings do not overtly support these diagnoses. Again, the reason for such practice revolves around many patients either unwilling to or unable to pay for diagnostic tests and then having to spend more time and money to return for follow up afterwards.


As for prenatal patients, most will have a first and second trimester ultrasound for dating and anatomy screening, and the usual prenatal labs. Every patient receives a tetanus booster and one dose of anti-parasitic medication during their second trimester. Fetal heart tones are assessed with a stethoscope through the patient’s abdomen, and feeling the location of the fundus assessed fetal growth. Fetal presentation is assessed by palpation and only assessed by ultrasound if the physician did not feel confident about palpating the head in within the maternal pelvis. Elective primary cesarean sections are quite common due to fear of labor pain, since pain management during labor is not available at this particular hospital. If a patient complained of contraction pains between 39 to 40 weeks, they were often admitted to the hospital for observation overnight and then induced if they did not progress into labor spontaneously. Again, this common practice is due to lack of access to medical facilities and the inability for patients to return repeatedly for labor checks. For these reasons, evidence-based medicine was rarely practiced.

There were two operating rooms that were separated by a glass wall, thus patient privacy was non-existent. Everyone in the operating room changed into scrubs and “OR slippers,” thus toes remained exposed. Those that scrubbed in wore fabric gowns and masks without any protective eyewear. Equipment that is normally disposed of were “sterilized” and reused, such as suction tubing and MVA cannulas. Makeshift baby warmers were put together in the OR during cesarean sections with a portable electric wire-grated heater directed onto baby blankets and towels. Almost all patients received 5-7 days of broad-spectrum antibiotics postoperatively regardless of the type of surgery they received due to the sanitation conditions and overcrowding of the inpatient wards. During times when the scheduled daily power outages were in effect mid-procedure and the power generator had not kicked in yet, we would continue the operation under guidance by flashlight. When a patient presented for a cesarean section, there were no baby warmers in the OR. Instead, a large portable metal heater propped up on a table pointing towards blankets and towels to be used for the delivery became the makeshift baby warmer. What I learned the most in the OR was how to be as least wasteful as possible since the patient has to purchase all of the materials used during surgery. Instrument tying was used to conserve suture, gauze was rinsed with warm saline and wrung out to be reused for dabbing blood.
One of my most memorable and rewarding experiences is from the free women’s health clinic hosted by us medical volunteers through the Mountain Fund at a local daycare center/school named, “Orchid Garden.” This daycare center is a very special one because it was built from the vision of a woman named Bina Basnet, who did not want children to be abandoned, but to have a place where children will be safe, well taken care of and educated while their mothers were at work. Thus, she became the founder of Orchid Garden, which is a non-profit center that accepts children from the age of 6 months to 8 years, and with classrooms from pre-K to grade 2. In total, there are almost 900 children at this center, with 150 children that attend grade 3 at outside schools from funding through the Orchid Garden. At the women’s health clinic we hosted, we saw and treated over 35 women for various conditions such as dysmenorrhea, menorrhagia, vaginal itching, abnormal discharge, abdominal pain, and pelvic organ prolapse. Those that required inpatient evaluation were referred to Helping Hands Hospital. Our exam rooms consisted of two school desks covered with sheets and a mini-mattress, with the two exam tables separated by a bedsheets tied to support beams near the ceiling. Our speculums had to be soaked in a sterilization solution for 45 mins before use on the next patient. The staff from Orchid Garden and local Nepali girls from the Mountain fund served as our translators. Because of the language barrier, each patient took at least 30 mins to assess. But, in the end, the patients were extremely grateful of our services and left with ear to ear smiles with free medications appropriate for their condition which they otherwise would not have been able to afford.
Words can only partially describe how rewarding and fulfilling it was to spend an extended period of time practicing medicine in a developing country. I feel so blessed to have had this opportunity during my residency training to go abroad for an educational experience. It has allowed me to reflect on how fortunate we are to have the resources we have to provide such advanced quality of care for our patients here. I have also learned to appreciate the fundamental things that we have that I surely never thought twice about before—adequate lighting, running water, protective personal equipment, private patient rooms, disposable equipment… and the list goes on and on. If I have the opportunity again to go abroad and provide medical care, I would jump at that chance as it is nothing short of a unique experience that offers insight on the world and within oneself. This experience has also reminded me of the reasons why I chose a career in medicine, which has strengthened my personal mission to provide the most compassionate care I possibly can as a doctor, and as a human being.


“Good very good fortune obtaining people powering this just one distinct. However you make some Really interesting aspects, youre likely to need to do way more than deliver up a pair of things which may be different than what weve presently read. Exactly what are aiming to say suitable below? What would you want us to imagine? It seems such as you cant definitely get powering a particular assumed. In any case, thats just my look at.”
Enoch Ginnis http://www.myexoticwife.com/members/suzannabe.5194/
Very good information. Lucky me I came across your site by accident (stumbleupon).
I have book-marked it for later!