Written by Tuong Van Nguyen, MD, PGY-3 at Kaiser Permanente Santa Clara Obstetrics & Gynecology…
Guatemala – Hospital de la Familia
Posted by Christopher Tang, MD (a fourth year Head and Neck Surgery resident from Kaiser Permanente, Oakland while on a global health elective in Guatemala with Hospital de la Familia ).
Pre-Trip Thoughts
My name is Christopher Tang and I’m currently a 4th year head and neck surgery resident at Kaiser Oakland Medical Center in Northern California. I’ve always been interested in mission trips and going to 3rd world countries and pursuing a mission there. I think all physicians have a unique capacity to reach out and extend ourselves to those in need through all cultural and linguistic barriers, since everyone, in the end, is still human with human medical problems. I’ve gone on medical missions in the past as a medical student: 2 trips to Mexico, and a 2 month trip to China, however, haven’t been on one since receiving my MD. Residency has been too busy and I never had the opportunity to leave my clinical duties. About 3 weeks prior to my Guatemala trip, I found out that one of my co-residents a year below me, would be unable to attend the trip since she was pregnant. She asked if I would be willing to go, and of course, I jumped at the opportunity to go. It was a little difficult to get everything organized, and cost a little extra buying the airfare at last-minute, but it all worked out great. In addition, I was accepted for the Kaiser Permanente Northern California Residency Program Global Health Program, which helped provide a large proportion of the funding necessary for the trip. Without the funding, I don’t think I would’ve been able to go and experience such an amazing experience. My pre-trip expectations were completely blown away and little did I know I was about to embark on an experience that is both eye-opening, and potentially life changing.

September 12th – Packing day
The day prior to departure was a normal day at Kaiser Oakland Medical Center. I was the acting chief resident of the service as the current chief was at a conference, so was taking care of things on the service, seeing patients, operating. I did 3 parathyroid surgeries and a vocal cord injection prior to leaving. After work, around 7PM, I gathered some equipment from the clinic such as a light source and our trusty nasopharyngoscope and I drove to Walnut Creek to pack it and place it in boxes there. I couldn’t believe it but when I got there, there was a truck with around 60 huge boxes of medical supplies. These were all going to be shipped to Guatemala with us. Basically on the trip we were allowed to carry on our own personal belongings, and the 2 luggage/baggage was used for the medical supplies. We talked to our director of operations, Diane Nishikawa-Solomon, and received instructions for the next day.
September 13th– Travel day
It would be a rough night since we had to arrive at SFO by 4AM to help unpack all the boxes and get them through to the airline. My friend Rebecca, the OR tech came and picked me up around 3:15AM, and then we picked up Dr. Hilsinger (chief of our department) at 3:30AM at Kaiser Oakland and drove to SFO. We left SFO around 6:50AM, and arrived in El Salvador around 1PM or so. There we met the rest of our team, and around 35 people gathered together. There was a team of ophthalmologists and optometrist who would set up an eye operation (with optometrists to give out classes, and ophthalmologists performing cataracts). They would perform roughly 30 or 40 cataracts a day for an entire week.

There was a general surgery team consisting of 2 general surgeons and a 4th year general surgery resident. They would do many hernias and gallbladders. There were 2 plastic surgeons (one general plastics, and one hand) who would do cleft surgeries there. And finally there were all the ancillary staff who would help us see clinic patients, circulate for us, and prep and support us.
We left El Salvador around 2PM for Guatemala City. When we arrived at Guatemala City, our medical equipment was shipped to the hospital while the rest of us boarded a bus for a hotel. It was around 5PM and we would stay a night in Guatemala City before departing at 6AM the next day. That night we went out to eat at hacienda de la real and got some good Guatemalan food. I got a chance to talk to the other staff not from our department and really enjoyed spending time as a group. We had a good meal and that night stayed at a hotel. We would get a wake up call at 5AM, breakfast at 5:30AM and then off on the road at 6AM.
September 14th (Friday)
Drove to Nuevo Progresso. The trip to Nuevo Progresso was a rough one. During the trip there was an accident on the road and the road was blocked for a few hours. (below) It was a very hot ride as there was no AC on the bus and ventilation was poor.

After about 6 hours we stopped at supermarket and bought some supplies for the week. I bought a pillow and it was really great to have A/C there again. We finally arrived at the hospital around noon, and then saw clinic patients. We signed up 3 patients for OR the next day. Clinic was very basic as we didn’t have a lot of equipment. Instead of sterilizing we had to clean everything with alcohol. Very interesting way how they do things.
Nuevo Progresso was located in the middle of the jungle in the mountains. After driving for 5 hours, we had to go an additional hour by dirt road to get there. The situation there was very unique in that the hospital was funded by the families club in San Francisco and was connected with a catholic convent there. Four to five times a year there would be mission trips to the hospital where surgeries would be performed with teams of around 50 people there. In the meantime, Guatemalan doctors would be there to act as primary care physicians and to provide continuity.
September 15th (Saturday)
Busy day… well they all were. On the first real day there we got to work right away. As we were there to operate and work, that’s what we did most of the day. We would wake up around 4AM everyday to the roosters and get ready for the day.
At 6AM people would start lining up and getting registered for the clinics. Hundreds of people would come everyday (above) and some even came from Mexico down to see the physicians there. Often they would drive there with their village since it would be such an ordeal to get there. Everyone would show up at 6AM, and we would see them throughout the day. Often people would get there at 6AM and then wait all day to be seen by us at 5PM. Since there were so many people we’d only get roughly 10 minutes for each patient.
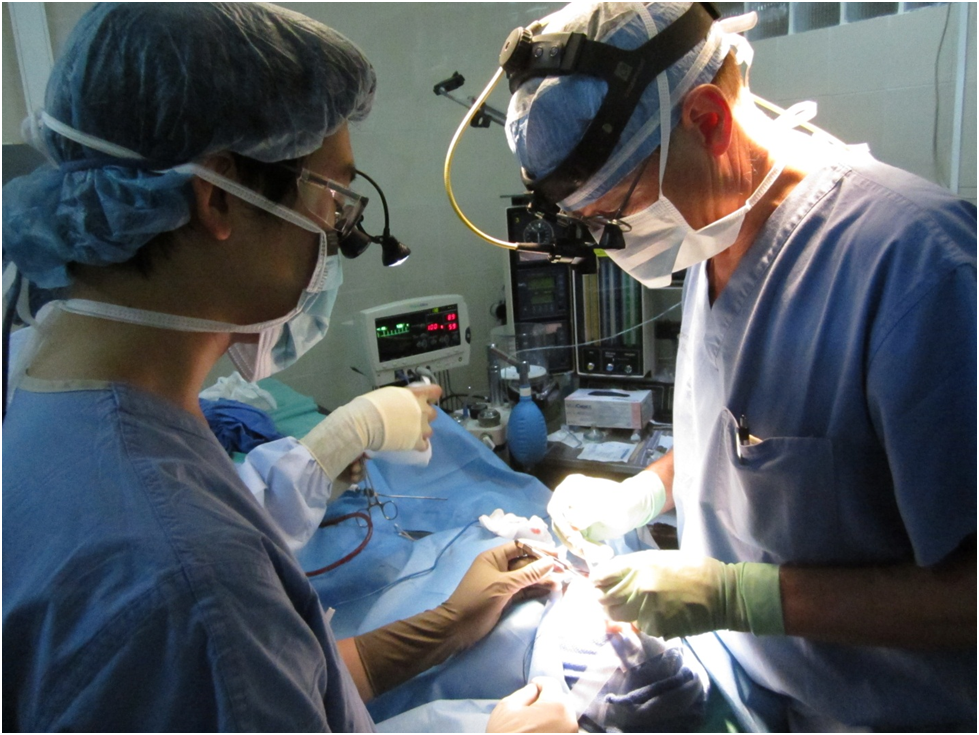
The OR there was very interesting. There was a large room with 4 operating tables in it where we would spend the majority of the day (below). There was a supply room that contained items from previous missions since this project has been ongoing for many years now.
On Saturday I went to OR, did 3 cases and then saw patients in clinic. Here’s a brief summary of the 3 patients I saw.
- Tonsillectomy on a 8 y/o kid. Performed it with bovie since coblator was not available. Mirror had no FRED anti-fog so was difficult to see, but was able to use his spit as a defog. Did not do adenoids because there’s no adenoids
- Kid with EAC cerumen impaction. Unable to be cleaned out and remove in clinic. Patient had hx of submucous cleft palate s/p repair with furlow palatoplasty with good outcome. Patient had poor hearing and developmental delay (speech delay). Removed cerumen so patient can get audio exam tomorrow.
- 12 yo F with R tympanic membrane perforation from umbo down to inferior annulus. Repaired with underlay graft made with temporalis fascia. There was a bug in our antibiotic solution. Just shows how things are entirely sterile down there. No floxin was available in the OR so we used IV kefsol and applied it topically. Found ophthalmologic floxin later and gave it to the patient. Microscope was very abnormal since it was an ophthalmologic scope and at a weird angle.
After OR I went back to clinic to help out. In clinic I saw a 17 yo girl in clinic with a R canal atresia and small ear. I would have liked to repair it, but unfortunately we didn’t have access to a CT scanner, so I would have no idea where the facial nerve is. It would be really difficult to perform a canalplasty so unfortunately we couldn’t create a new canal for her. Also, since we didn’t have the facilities or the capability to do a multi stage ear reconstruction with rib cartilage (4 stage Brent method), we had to tell her it couldn’t be pursued. She was very sad and cried since she waited so long to have it done and really wanted to.
That day also happened to be Guatemalan Independence Day so all day there was marching and a band playing while I was operating. We had dinner in our common room and then rounded at night. It was a very simple life. No internet, no phone.
September 16th (Sunday)
Went to OR again. Each day was about the same and worked something like this. Wake up at 4AM from the roosters. Breakfast at 7AM. Rounded on our patients that we worked on around 7:30AM. Started operating around 8AM. Finished around 7-9PM. Had dinner then. Rounded at 10PM. Slept around 11PM. Repeat. A few things of note on Sunday.
- Tonsil kid bled overnight. I felt really bad about this since I had come here to help him and he ended up bleeding. I had a talk with my attending about it and he told me not to feel bad about it, but just realize that complications do happen. The key is not to minimize things, but to realize that they did occur and do the right thing to fix it. Bleeding after tonsils is a given complication. We brought him back to the OR. Stopped the bleeding. Cleaned him up and he was fine and went home the next day. I learned a valuable lesson that day about not feeling bad about complications, but instead realize it and fix it.
We helped fix a guy with a hernia the size of a basketball in his scrotum. Basically his intestines have fallen into his scrotum and we helped him repair it. There were a lot of hernias to be done in the 3rdworld since there was a lot of manual labor and doing such increases intrabdominal pressure and causes things like that to happen. I also helped out with a kid with a bilateral cleft lip and palate. I did the bilateral cleft lip with an excellent plastic surgeon from San Francisco. It was an amazing surgery that took a long time to perform. It was hard to close the orbicularis muscle around the premaxilla, but afterwards, we were well satisfied. That afternoon I rushed through PM clinic. We saw a ton of patients. I also saw a patient with rhinophyma. We decided to schedule the rhinophyma patient for OR. We shaved off his rhinophyma and cauterized the base. He will re-epithelialize in no time.
September 17th (Monday)
I had clinic all day. We ran out of O2 in the morning so ended up going to OR really late (around 11AM), and then finishing late (around midnight) since we had so many surgeries to be done and not enough time. That night we took out a huge sebaceous cyst from a guy’s scalp. It was the size of a tennis ball.
September 18th (Tuesday)
OR all day. Had breakfast at 7AM, started at 7:30AM, finished at 7PM. Did the following
- Tonsil – holdover from yesterday. Tonsil in 8 yo kid. Removed tonsils. No bleeding
- Submandibular gland excision for chronic sialadenitis. With Dr. Wang. Went well. Identified both lingual and hypoglossal nerves. Learned new ways to do it
- Septoplasty – Bled in PACU, so packed with 8 cm merocels. People seem to bleed a lot here. Turbinate outfractured. Later she would be re-packed with larger merocels because of bleeding.
- Sinus surgery without a scope! Amazing! Did it with Dr. Hilsinger. SMR of bilateral inferior turbs, and then removed polyps from middle meatus bilaterally, medialized middle turbs, and then made maxillary antrostomy bilaterally. It was interesting to see how they did it in the old days. The patient did great afterwards. No complications. Good vision.
September 19th-20th (Wednesday and Thursday)
Wednesday I operated all day again like the previous days. Sadly, Thursday morning I had to leave back to California. The rest of the group was going to stay until Sunday, but since I booked the trip late, I already had previous engagements and wouldn’t be able to stay. Thursday morning after rounding I left the hospital with one of the general surgeons. We paid a guy to drive us back in his pick up truck. The ride was 6 hours back to Guatemala City. Then took a plane back to El Salvador, and then back to California, arriving at 1AM in SF. We were travelling for roughly 16 hours. What an amazing, life changing trip.
Post trip thoughts
In retrospect, I wish I could’ve stayed longer and have done more. Unfortunately we only had our limited man power and limited medical supplies. Since most people have to take vacation time to go on these trips, there just isn’t enough time for us healthcare professionals to have time to do these missions. There is just so much work to be done and not enough time to do it. I would’ve also liked to have spent some time walking around town, or visiting places. I literally just worked the entire time I was there. I wish I had some time to talk to people in a non-medical capacity and learn about the culture a little more in that way, or explore town a bit, but since we were up by 4AM and went to sleep at 11PM everyday operating and seeing clinic patients, it was difficult to even have time for meals. If I could do it again, I would’ve stayed longer and in addition to doing all the clinical work maybe take some time to see the surroundings a bit. Nonetheless it was really eye-opening to see what people have to go through and the lack of medical care in these villages.








I’m amazed, I must say. Rarely do I come across a blog that’s both educative and entertaining,
and without a doubt, you have hit the nail on the
head. The issue is something which too few folks are speaking intelligently about.
Now i’m very happy that I found this during my search for something regarding this.