Written by Hongyu Zhao, MD, PGY-2 and Qing Meng Zhang, MD, PGY-2 at Kaiser Permanente…
Complications
7/30/12
Posted by Amanda Thornton, MD (a third year Internal Medicine resident from Kaiser Permanente, Oakland while on a global health elective in Lusaka, Zambia with University Teaching Hospital).
Today I had my first “Major rounds.” On major rounds, the attending physicians, here called “consultants,” go around to each patient admitted to the Medicine service in the hospital and discuss their case at the bedside. They do this with the team 2 days of the week- the male ward on the first day, the female ward on the second. This means they take their time on every patient and our discussions ran from 8am to nearly 2pm. The rest of the week, the interns see every patients and make medical decisions on their own. One of the interns admitted she had seen 24 patients today- which is very different from the limited numbers of patients interns are allowed to see in the United States. I have only seen a maximum of 16 patients a day, and that in the second year of my residency; when I asked if I could see patients with her, she said she would be grateful for the help.
Patients who survive to sit in a hospital bed here are often relatively stable- but the patient I had been assigned yesterday to present this morning had passed 30 minutes before I arrived. She was a 26 year old widow with AIDS and did not have the funds to pay for the high cost ward. Though she had been faithfully taking anti-retroviral therapy for three months and had initially improved enough to take a part time job, she had started to feel overwhelmingly weak 2 weeks before she came to a community hospital. From the community hospital she had been referred UTH for further work up.
When I saw her yesterday, she was surrounded by visitors and was very easily tired from the effort of answering my questions. She told me to come back tomorrow so she could tell her story. She had been losing weight from the time of her diagnosis 3 months ago, and I was very worried that she was suffering from AIDS associated wasting. It sounded as if her infection had not responded appropriately to the highly active anti-retroviral therapy (HAART) she had been prescribed. Involuntary weight loss in advanced HIV infection can be caused by a combination of many different conditions, but it is associated with lower CD4 counts (one of the parameters doctors use to gauge a person’s response to treatment for AIDS and their ability to fight serious infections associated with AIDS) and increases the patient’s chances of dying despite appropriate treatment. She told me that she had felt worse and worse every day she was in the hospital; I was sorry that we could not have helped her more.
It is amazing how much clinicians here have to rely on clinical findings- the physical exam and history of illness the patient reports. In the United States, I have heard residents say that eventually the physical exam and history will be obsolete, and the appropriate interpretation of a battery of tests will be all that is indicated in order to diagnose and treat patients. After having been here for just 2 days, I am even more firmly convinced that it is important to continue to learn how to elicit an accurate clinical exam to be a good and effective doctor. Here the physicians have no other choice- Laboratory exams are expensive and usually take 1-2 days to come back. Imaging is also difficult to schedule and have performed; ultrasounds are read by technicians rather than radiologists, and physicans, like the team’s attending Dr. Mukomena, read imaging at the bedside and use it to directly support the patient’s diagnosis so that treatment is started immediately. The untreated patient has not been helped, he explained to the team, and they come to the hospital for treatment.
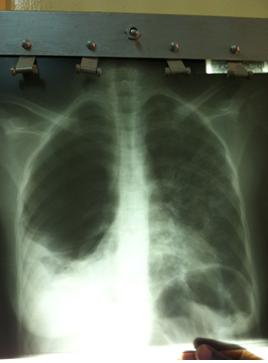
For example, today, we had a discussion about a patient with incompletely treated tuberculosis (TB) and HIV who presented to the hospital two days before with shortness of breath, chest pain and hypoxia. She had not improved despite starting treatment for TB and supplemental oxygen. Her X-ray had been performed the day before. We all looked at it in the light of the window, but on listening to the patient’s lungs, Dr. Mukomena called all of the learners on the team to listen at a particular spot on her chest.
“Listen, do you hear it?”
“Almost a whistling?” I asked after listening to the spot he indicated.
“No, not whistling. Like the sound you hear when blowing over the top of an empty soda bottle. Amphoric breath sounds. She has a pneumothorax or a large cavitation.”
The team assembled a needle with a syringe of sterile water, and he inserted it between her ribs, and drew back. “You see the way air comes out and bubbles through the water? There is air outside the lung- she is only breathing with her other lung, this one is not being used.”
We re-examined the chest X-ray on one of the few light tables in the ward (see below)- we had to unplug where a patient had been charging her cell phone before we could plug it in and turn it on. He outlined the large space where he hypothesized that either tuberculosis gradually had eaten away at the lung tissue to form a large hole in the parenchyma (a cavitation) or it had damaged the lung enough for a pneumothorax to form. The intern wrote for a surgery consult for possible chest tube placement and the team moved on.
This afternoon, I went to the library to investigate TB complications that I was simply not familiar enough with given my experience in treating an American population with relatively low rates of TB. The library was full of medical students and physicians who were “revising” (what they call studying) for major rounds or for exams. Internet bandwidth is limited, and I have not been given access for my iPhone. Today, the desktop computers’ internet was not working at all.

I found a book entitled “Tuberculosis: A comprehensive clinical reference” (Schaff/Zumla) which reported that pneumothorax is a very rare complication of untreated tuberculosis, only 5% of patients with severe cavitary disease will develop one. Two patients on the service have another complication of TB rarely seen- constrictive pericarditis, on which I read a chapter. Already, I have so many things to learn and I expect I will be coming to the library very frequently the entire time I am here.
Now, two days off before I start in the hospital’s outpatient clinic on Monday. This weekend, I plan to try and connect with Americans here and start a membership in a nearby gym. Next week I will be accompanying Dr. Mukomena to an outpatient clinic he staffs in an underserved area near Lusaka.
This Post Has 0 Comments