Written by Deepika Parmar, MD, PGY-2 at Kaiser Permanente Oakland Pediatrics Program while on Global Health…
My Matibabu Experience
Posted by Ganga Madduri, MD (a third year internal medicine resident from Kaiser Permanente Oakland serving a global health elective at The Matibabu Foundation in Ugenya, Kenya).
4/21/10
I became a doctor in order to contribute to international health, and thus I have very broad interests when it comes to medicine. Although I am an internal medicine physician, I know through experience that you cannot limit yourself to just adult medicine when trying to participate in these efforts, and so I asked to do surgery and pediatrics in addition to the outpatient clinic already established by Matibabu. The Matibabu Foundation was started by Dr. Gail Wagner from Kaiser Permanente in Hayward and Daniel Ogola, a very hard working and bright man who grew up in Ukwalla, Kenya. Kaiser Permanente physicians have been volunteering through this organization since 2003, and luckily for me it was opened up to residents this year, my last year of residency. This was my second time volunteering in Kenya, so I knew a little bit of what to expect.
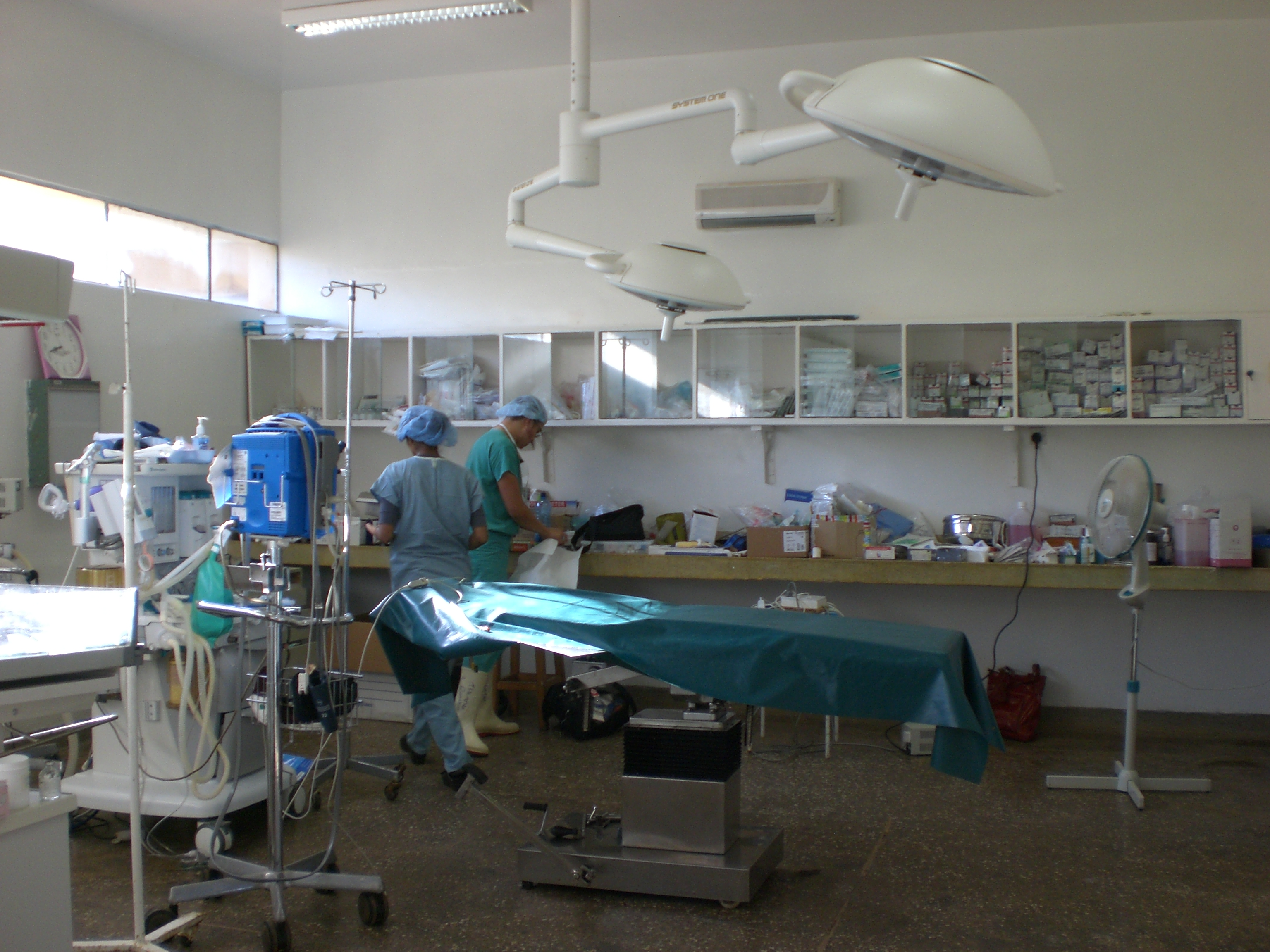
When I got to Siaya, the surgery team from Kaiser Hayward and San Francisco had already been working for one week. It really was a complete team including 2 surgeons, 1 anesthesiologist, a scrub nurse and PACU nurse. They were using the Siaya government hospital OR and some staff for scheduling surgery. By being able to participate in surgery, I learned the challenges faced by surgeons coming to a developing country and providing their services. There were 2 OR rooms adjacent to each other, and depending on the time of day, the surgeons would practice in the room that the sun was currently shining into – when the sun was setting, they would switch to the opposite room. Just recently the rooms received operating lights so fortunately doctors do not have to practice by just sunlight anymore. The surgeons brought an impressive amount of medicines and equipment (anesthetics, betadine, gloves, surgical instruments, vital sign monitoring equipment, etc.), but things were still challenging. For example, the idea of post anesthesia care does not exist there in that rural government hospital. As a result, Julie, an ICU nurse from San Francisco, was trying to teach the nurses there how to monitor a patient after they have come out of surgery and make a smooth transition to the wards without any complications. However, I realized quickly that we can’t force change or teach change just because we come into their lives and are volunteering for two weeks when this is the way that they have always been practicing.
After the surgery team left I transitioned over to the Matibabu Ukwalla clinic. I stayed with a wonderful Kenyan family and walked to the clinic everyday. This family was well known to the Matibabu members and several volunteers have stayed with them before. The tribe that lives in this area are called the ”Luo”, they are polygamous by custom, and have a different dialect than Swahili. So I was able to learn some Luo terms as well as some Swahili words to converse with my patients. At the clinic, I felt frustrated with some practices: antibiotics were given out like candy to anyone that had a cough, even after I tried to explain to the medical officers whom I worked with that not everyone with a cough had bacterial pneumonia. In addition, elderly patients with osteoarthritis were treated with frequent IM steroid shots instead of joint injections or NSAIDS and Tylenol which is the standard of care back home. I tried to teach them the many adverse effects of systemic steroids especially in an environment with immunosuppresion and prevalent HIV.
The Matibabu Foundation members, Dan, and the multiple Kaiser attendings I worked with (Dr. Ramachandran, Dr. Sherris, Dr. Godfrey) kept in touch with me frequently to make sure my accommodations were okay and that my experience was worthwhile. The patients and other Kenyan locals I met were very warm and welcoming. I really enjoyed working with other medical officers in the clinic. I was grateful to the young man who translated for me, Dan (not Dan Ogola), not only for his time but also for his knowledge. He taught me so much about the beliefs of the Luo people because he was Luo himself. He wants to be a doctor as well so I tried to teach him as much medicine as I could while seeing patients in clinic with him. Teaching is my first love, even before medicine, so it was a pleasure to have him there so eager to learn, and I hope he does end up finding work in the medical field. I spent one week at the outpatient Matibabu clinic where I primarily saw malaria and amebiasis. I also sharpened my ultrasound skills from seeing women with abdominal/ pelvic pain. I learned that African women more frequently suffer from fibroids with subsequent pain requiring hysterectomy. From Ukwalla, I traveled with my attending, Dr. Peter Sherris, to the lively and active town of Kisumu where I would be volunteering in the Kisumu District Hospital, a government hospital (KDH).
At KDH, I participated in several different activities. In the pediatric wards, I rounded with the wards teams which consisted of several medical officers in training (comparable to our physician assistants) and one attending. The ward had approximately 15 beds, each bed held approximately 3 pediatric patients and also their mothers who were responsible for feeding and cleaning the children. One day during rounds, we found a 5 month old child in shock that had come in the evening before with dehydration and diarrhea. She was seen by one of these medical officers in training and had been given oral rehydration, though she did not get any lab tests because the lab is closed in the evening. However, for whatever reason the mother was unable to feed her through the night while the baby continued to have diarrhea. In the morning while we rounded on the baby she was unresponsive with very poor skin turgor and pale conjunctivae. A peripheral IV was placed and a rapid malaria test was positive. She was likely dehydrated from the diarrhea and hemolyzing from the malaria, yet the government hospitals did not have IV fluids at that time given that the Kenyan government had used up all its funds for the hospital for the next few months. To get around this problem, the family members are told to go buy the IV fluids and necessary tubing from a private pharmacist. As a result, the mother was sent out on this mission. While she was gone we discovered the baby didn’t have any pulse and had stopped breathing so CPR was started but did not bring back a pulse. We covered up the baby and moved on with rounds, and when the mother returned with the IV fluids, she saw her baby was completely covered by the blanket. She let of a loud shriek and dropped the IV fluids on the floor and started sobbing. I felt helpless and really wished there was something I could do. We had antri-retrovirals and anti-malarial drugs but no IV fluids which is thought of as such a simple and widely available treatment in a hospital.
While at KDH, I also spent time in the malnutrition unit and learned a lot about Kwashiorkor and Marasmus. I loved hanging out with the babies, and the nutritionist was so helpful by giving me some reading about the nutrition guidelines currently in place. There were several babies there who were there chronically. One with HIV and TB who had failed TB treatment and was chronically malnutritioned. I learned how hard it is to give good nutrition to a child with HIV and chronic diarrhea because everything you put it comes out so fast and in addition to diarrhea from HIV, the children get amebiasis frequently. I was surprised to learn that mothers who are HIV positive are encouraged to breast feed their babies. Studies in Sub-saharan Africa have shown that if replacement feedings are used instead of breast milk, the mortality from diarrheal illnesses in the first 6 months greatly increases, thus the benefits of breast feeding outweigh the risks in this environment.
One day during this week I went to visit the Aga Khan Hospital (AKH). I had never been in an Aga Khan facility before, so I was shocked at the change from the government hospital where I had been working. AKH had a CT scanner, a talented radiologist who did Echos and insertion of subcutaneous drains, private patient rooms and bathrooms. It was actually nicer than most hospitals I had been in back home, and at AKH, I met residents in training. One resident was researching Pulmonary Hypertension in HIV by doing Echos on all their HIV + patients. He was finding that their incidence was 3-4 % which is much higher than the incidence in the western countries (0.5%). I found it extremely interesting that a virus can cause pulmonary HTN, and I was puzzled by the idea that HIV in Sub-Saharan Africa can cause more of this pulmonary disease process. One of the reasons I was visiting the AKH was because Matibabu is trying to set up some affiliation such that they can see our patients in Kisumu if our patients need CT or ultrasound and we can see their patients in Ukwalla especially when we have specialized surgeons from the US rotating through.
In the end, I feel extremely fortunate to have had this opportunity to experience so many different health care settings abroad: clinic in rural setting, surgery, pediatrics and HIV clinic at a government hospital, private hospital with residents in training. I was so impressed with the attendings I met on this trip who all do so much more than just volunteer. For example, these people routinely acquire significant funding and make contacts with people such as the Kenyan president and ministers. That there is no religious affiliation and everyone is treated was also very attractive to me. I hope in the near future I will be able to go back and find more ways to contribute.


This is fabulous for the great concern that matibabu has towards creating medical awareness and bringing lucrative services to the poor not only in ugenya but also in entire kenyan region.Bravo and may the Almighty God strengthen you all in the matibabu foundation for realisation of more objectives.Let matibabu rise to greater heights.